Our analysis
Introduction
Each month in our NHS activity tracker we consider the national data and look across physical and mental health services to see what care the NHS is delivering, what is happening to waiting lists and how the NHS is performing against existing waiting time standards. We will also examine the ongoing pressures and challenges for trusts as they help staff recover from an unprecedented year, and address the care backlog. We will also feature case studies from trusts to highlight the important work they are doing to adapt, improve and innovate in the face of the constantly changing clinical and operational environment.
As a direct result of the national lockdown measures, the COVID-19 pressures in many hospitals have started to ease in recent weeks. We have been tracking the trends in our daily dashboard.
As of 10 March, there were 6,975 COVID-19 patients in hospital –down from 34,336 patients at the height of the latest peak on 18 January. However, although nationally the number of patients in hospital is reducing, the NHS is still using additional surge critical care capacity, with 16% of all COVID-19 patients in hospital currently in mechanical ventilated beds.
Positively, infection rates are falling in the community and the NHS in England has administered over 20 million vaccines - with 34.4% of the population now having received their first dose.
This month’s performance figures
Each month NHS England and NHS Improvement publishes statistics looking at performance across a range of services including urgent and emergency care, routine care, cancer, and mental health. We have been tracking the trends in our daily dashboard.
Overall, and as a direct result of the national lockdown measures, the COVID-19 pressures in many hospitals have started to ease in recent weeks:
- As of 10 March, there were 6,975 COVID-19 patients in hospital –down from 34,336 patients at the height of the latest peak on 18 January. However, although nationally the number of patients in hospital is reducing, the NHS is still using additional surge critical care capacity, with 16% of all COVID-19 patients in hospital currently in mechanical ventilated beds.
- Positively, infection rates continue to fall in the community and the NHS in England has administered over 20 million vaccines - with 34.4% of the population now having received their first dose.
NHS 111 and ambulance: In February 20210 there was a slight dip in demand for NHS 111 and ambulance services:
- The number of NHS 111 calls offered in February 2021 fell by 16.3% compared to the previous month (258,961 fewer calls), also 18% lower than the same time last year. NHS 111 activity is around half of the levels observed during the first peak at the start of the pandemic.
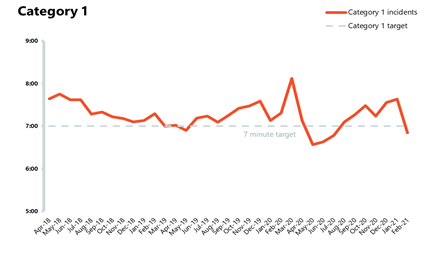
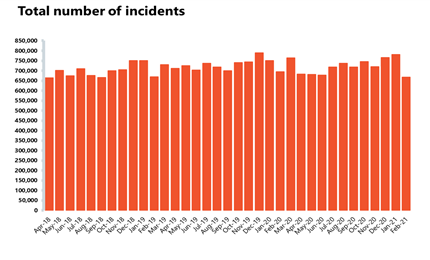
- The most serious category 1 incidents decreased by 20.4% to 49,231 in February – meaning there were 12,596 fewer incidents than in January. In comparison to the same time last year, so before the pandemic, incidents are down by 13.1%. The fall in activity across the urgent and emergency care pathway, including in A&E is most likely, in part, a result of the ongoing national lockdown restriction.
- In terms of performance against the ambulance standards, the mean average response time across England in February 2021 for category 1 calls was 6 minutes and 51 seconds, meaning the service met the 7 minutes target for the first time since July 2020. The average response time for category calls has improved significantly and only slightly missed the 18 minutes target with a national average response time of 18 minutes and 19 seconds. In January 2021 when we know the pathway was under immense pressure the average response time was (29 mins 40 secs) and a significant improvement than the peak in March 2020 (32 mins 6 secs).
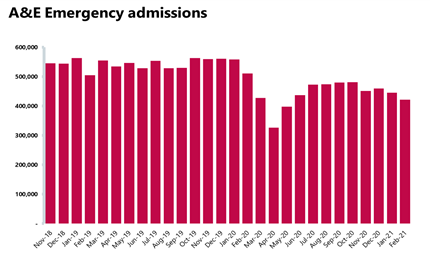
A&E and emergency care: The lockdown continues to impact emergency care activity.
- This month’s data shows congestion in A&E’s easing. In February 2021 there were 1.28million A&E attendances – a reduction of 2% on the previous month, and 35% fewer than a year before the pandemic in February 2020. However, critically, A&E attendances have not fallen to levels seen in April 2020 and remain 39% higher with admissions 29% higher than in April 2020. Emergency admission also fell by 5% from the previous month and continue to be 17% lower than February 2020.
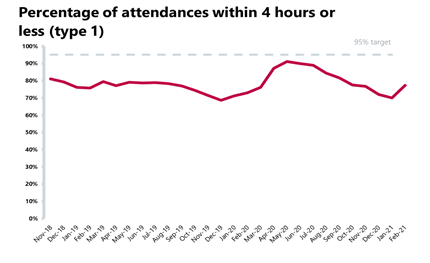
- In February, 83.9% of patients were seen within four hours across all types of A&E - an improvement of 5.4 percentage points on the previous month. However, the proportion seen within four hours is lower than observed in April 2020 in part because of the reduced activity levels during the first wave. The number of patients waiting longer than four and 12 hours from the decision to admit to admission have both fallen this month, after significant rises in the previous three months over winter.
- The number of people waiting longer than four hours has decreased by 40% falling to 57,169. Those waiting over 12 hours has also fallen by 73% since last month to 1,038 trolley waits, and numbers remain 36% below last year.
Elective care: In January 2021 there was a reduction in elective activity due to the ongoing COVID-19 pressures, resulting in a slight deterioration in performance against the 18 week standard and an expansion of the waiting list.
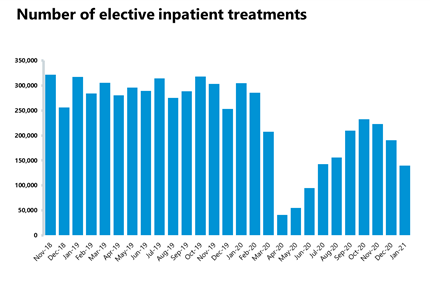
- Although elective care activity declined in January 2021, the number of inpatient pathways completed was still 239% higher than in April 2020 showing that the NHS did continue to deliver more elective care in the latest wave. This is no mean feat considering the NHS treated considerably more COVID-19 patients in the latest wave compared to the first peak.
- Of real concern is that fact that in January 2021 the size of the elective care waiting list increased by 71,342 to 4.6 million - a 1.6% increase on the previous month. The waiting list is bigger than it has been in over a decade, when data reporting began. However, the waiting list hasn’t expanded as quickly as some predicted, with a 4% expansion (175,255 more patients) compared to a year ago before the pandemic. This may be due to a drop in people seeking care but GP appointment data shows primary care activity is back to pre-pandemic levels suggesting that the pipeline of patients may have been restored.
- Performance against the standard declined since last month, with 66.2% of people on the waiting list currently under 18 weeks. Performance against the standard is still significantly higher than the all-time low of 46.8% in July and 53.6% in August.
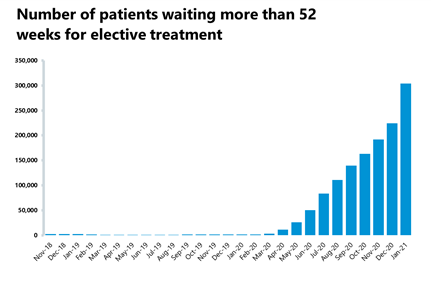
- The number which is most concerning to trust leaders is the number of people now waiting over 52 weeks: 304,044 people on the waiting list have now waited over a year for treatment, upby 35.6% from the previous month and considerably increased from the same time last year.
- In January 2021, the NHS delivered 139,378 completed inpatient pathways, a reduction of 27% on the previous month. Compared to the previous year the NHS delivered 54% fewer inpatient pathways, so roughly around half of usual activity. Trusts also delivered 822,218 non-admitted pathways, only a 2.6% reduction on the previous month, but still 29% fewer when compared to the previous year. However, the number has increased by 56% since the low in April 2020, again showing the NHS delivered more non-COVID care in the January 2021 peak than in April 2020.
Diagnostics: The backlog in diagnostics continues to be concerning. NHS performance falls short of the standard which states that 99% of patients should receive their diagnostic test within six weeks.
- In January, 33.3% of those on the waiting list had been waiting six weeks or more for a test, up from 29.2% in the previous month.
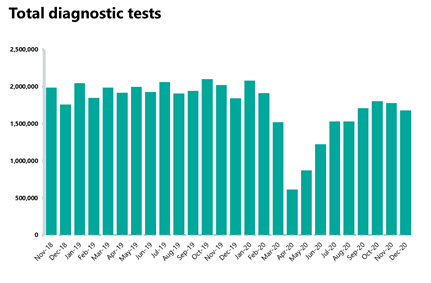
- There have been a total of 1.61 million tests carried out in January 2021, which is 4.1% fewer than the previous month and35.1% fewer than this time last year. Performance is however much better than in April 2020, with almost a million more tests carried out in January (163% more tests).
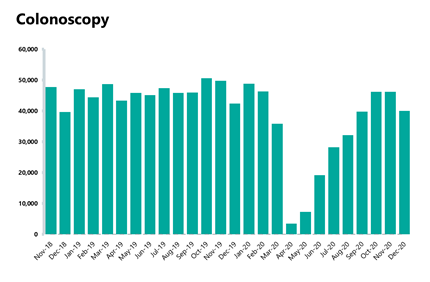
- The number of colonoscopy tests fell by 5.5% in January while CT and MRI were relatively steady since the previous month (-1.5% and -0.3% respectively). However, the number of colonoscopy tests is 35.7% lower than this time last year, with CT down by 16.7% and MRI are down by 29.7%. Activity has picked up considerably since the first wave in April 2020. Since then the NHS has carried out more colonoscopies, CT scans and MRI’s, +986%, +82% and +191% respectively.
Cancer: Similar to other services, cancer activity is down from the previous month, but holding up better than during the first wave. Performance against the standards has dropped considerably. The two-week pathway for a consultant appointment following an urgent GP referral has the worst performance on record this month.
In terms of activity and performance across the three key cancer pathways:
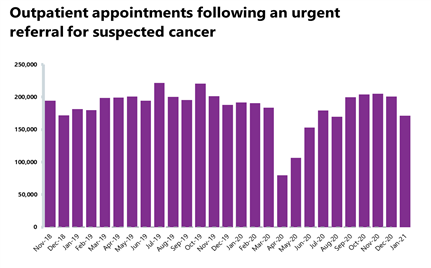
- 171,231 people had a consultant appointment following an urgent GP referral (two-week pathway), which is 14.8% fewer than the previous month (29,709 fewer). Compared to a year ago, this is 23% fewer than in January 2020 (20,621 fewer), but compared to the first peak in April 2020, this is 115% higher (91,658 more). Performance against the standard was 83.4%, down from 87.5% and missing the 93% standard.
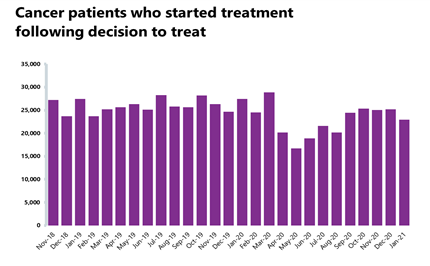
- 22,942 people started treatment following a decision to treat (31 day pathway), which is 9.0% fewer than the previous month (2,257 fewer). Compared to a year ago, this is 21.3% fewer than in January 2020 (4,522 fewer), but compared to the first peak in April 2020 this is 13.9% higher (2,805 more). Performance against the standard was 94.0%, down from 96.0% and missing the 96% standard.
- 12,438 people started treatment following an urgent GP referral (62 day pathway), which is 10.4% fewer than the previous month (1,442 fewer). Compared to a year ago, this is 17.8% fewer than in January 2020 (1,695 fewer), but compared to the first peak in April 2020 this is 15.3% higher (1,646 more). Performance against the standard was 71.2%, down from 75.2% and missing the 85% standard.
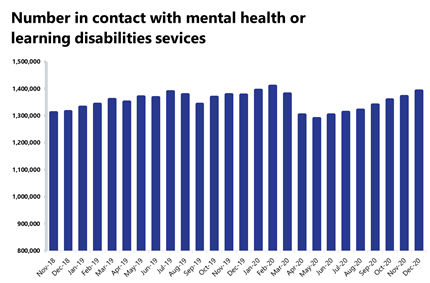
Mental health: In December 2020, the number of people in contact with mental health services continued to increase. During the first wave, the number in contact had fallen to 1.29 million in May 2020, but steady month-on-month increases since then means there are now 1.39 million in contact with mental health services, and this current total is now 1.1% higher than a year ago.
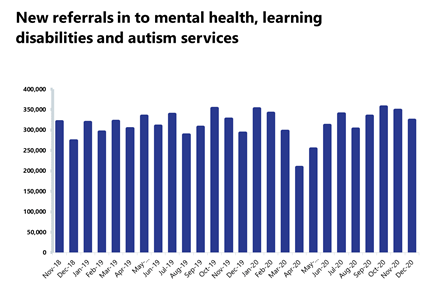
Some disruption can be seen in the number of people being referred for mental health services as the second wave gathered pace. In December 2020, there were 6.9% fewer referrals than the previous month, although the total of 324,580 for the month remains 11% higher than a year ago, and 55% higher than the lowest figure during the first wave in April 2020.
Our view
This month’s data shows that the NHS has had to adapt in response to the latest wave of the pandemic. The data clearly shows that although across many areas, activity has dipped slightly, there has not been a reduction in activity comparable to that experienced during the first wave. In fact, the NHS cared for 81% more patients in hospital at the peak of the latest wave when compared to the peak last April in addition to more non COVID patients.
Trust leaders are critically aware of the scale of the challenge ahead to address the care backlogs that span physical and mental health services and of the need to support frontline staff, many of whom are exhausted. Trusts will welcome the support of the national bodies and the government in prioritising and planning for the year ahead.
NHS activity tracker
A&E
Cancer
RTT
Diagnostic tests
Ambulance
Mental health
Case study
Epsom and St Helier University Hospitals NHS Trust: Emergency department capital investment
Daniel Elkeles, chief executive, and Dan Camp, divisional director for medicine and A&E, both of Epsom and St Helier University Hostpials NHS Trust, reflect on changes to their emergency department.
COVID-19 made us to reconsider the space in our emergency department. Our emergency and acute medicine teams had great ideas for working together in a new same day emergency care (SDEC) model but the emergency department configuration and separation of acute services compromised that vision. It was harder still once we considered the increased need for single rooms because of the pandemic. This meant our patients waited too long to see the right person or get to the right place, often in a waiting room where social distancing was very difficult.


Our estate in the reception area was limiting the effectiveness of the streaming process and compromising patients' privacy. Furthermore, our mental health room was heavily occupied and patients in crisis were being cared for in other parts of the department, sometimes noisy and chaotic areas.
An opportunity arose for capital funding to expand our emergency department footprint so we developed ambitious plans to extend into the surrounding areas. The increased space enabled us to think differently about the patient journeys and create new purpose-built areas that would support the models of care our clinical teams were aspiring to deliver together.
An opportunity arose for capital funding to expand our emergency department footprint so we developed ambitious plans to extend into the surrounding areas.
Chief Executive, Epsom and St Helier University Hospitals NHS Trust
The biggest change was creating an expanded purpose-built SDEC unit which delivered 12 additional spaces to be shared between ED and acute medicine so patients can see the right doctor first time rather than waiting for assessment or treatment. We also built procedure and examination rooms to support prevention of unnecessary admissions, and four single rooms for patients who may need isolation. Running a COVID-19 SDEC in the latest surge meant space in Majors and Resus was kept free for those who were sickest.
We created more waiting areas so reception became less crowded and patients could socially distance. We also created a separated streaming room with view of the waiting area. At the same time we implemented directly bookable NHS 111 appointments to reduce unexpected patients arriving. In designing the new mental health rooms, we worked closely with psychiatric liaison and security teams from our local mental health trust to ensure the best possible use of space for safety and patient experience. We have been able to double our adult and paediatric spaces from one to two whilst making the environment quieter and more comfortable with en-suite facilities.

By using modular buildings connected to the department, we were able to maintain co-location of key non-clinical areas immediately adjacent to the emergency department , to help staff to take their breaks and attend handovers.
The impact has been that our time to triage and assessment have consistently reduced and the number of patients who walk in to the department has decreased. These things have meant that our waiting rooms are less crowded, overall time in emergency department is lower than previously, and our four-hour performance has improved. Our SDEC activity continues to increase, although the overall time in the SDEC unit is being maintained at appropriate levels. Overall, the capital programme has been a huge enabler for new ways of working that deliver real improvements in safety and experience for all of our patients.
Overall, the capital programme has been a huge enabler for new ways of working that deliver real improvements in safety and experience for all of our patients.
Chief Executive, Epsom and St Helier University Hospitals NHS Trust
Press statement
NHS has a mountain to climb to clear care backlog
Responding to the publication of today’s performance statistics for the NHS, NHS Providers deputy chief executive Saffron Cordery said: "Today’s data reveals the incredibly steep mountain the NHS must climb as it seeks to clear the substantial backlog of care that has built up during the pandemic.
"The numbers are stark. More than 300,000 NHS patients have now been waiting for over a year for planned care with nearly 4.6 million people on the waiting list for elective treatment. We know these pressures are reflected across both physical and mental health services, whether delivered within a hospital, in the community or in people’s own homes.
"It is testament to the incredibly hard work of trusts and their dedicated staff that throughout January and February, they continued to carry out more consultations, operations, diagnostic tests, and cancer treatments than in the first wave, despite there being far more COVID-19 patients in hospitals across the country.
"But we cannot escape the fact, that with just 21 days to go before the new financial year starts, there is still no agreement on the NHS’s budget for next year. This begs the question of how trust leaders can plan frontline services, including addressing the care backlog, without certainty on their budgets.
"Talks between the Treasury and the NHS need to go up a gear and must be concluded this week. If they aren’t, there is a very real risk that trust leaders may have to start planning cuts of up to £7-8bn from NHS services from 1 April for the first half of 2021/22. Trust leaders need certainty now over their budgets and confirmation from the Treasury that any extra COVID costs they incur will be covered".