Our Analysis
Introduction
Today's test and trace data covering 27 May - 2 June 2021 confirms that cases of COVID-19 are increasing once again. 25,091 people tested positive for coronavirus in the latest week, up by 45% compared to the previous week. This is the highest weekly number of people testing positive since the week ending 31 March 2021.
Positive cases are beginning to translate into increased COVID-19 hospital activity, and as of Wednesday 9 June there were 876 people in hospitals across England with COVID-19. Some regions, such as the North West have been more impacted to date, but increases are now occurring across the country. However, pressure on intensive care remains low and the uptick in cases is yet to be translated into a rise in deaths. For more detailed data please see our daily dashboard where we track the latest trends for further detail.
Positive cases are beginning to translate into increased COVID-19 hospital activity, and as of Wednesday 9 June there were 876 people in hospitals across England with COVID-19.
The vaccine has provided hope that the link between infection and severe illness has been broken, but more time and data is needed to fully understand the impact of the recent increase in community prevalence.
Alongside the latest increase in COVID-19 pressures, trusts are telling us that demand has risen for mental health services, particularly for children and young people's services. Similarly, leaders are flagging the pressures across the urgent and emergency care pathway. This month, the national data presented in our NHS Activity Tracker supports what we are hearing, highlighting the widespread operational pressures the NHS is facing as we enter summer.
This month's performance figures
Each month NHS England and NHS Improvement publish statistics looking at activity and performance across a range of services including urgent and emergency care, routine care, cancer, and mental health. Below we set out the latest trend for each clinical area:
NHS 111 and ambulance
Activity has increased across the urgent and emergency care pathway, which is borne out in the statistics for NHS 111 and the ambulance service.
- How NHS 111 data is published has changed meaning data is not comparable to previous months. However, in May NHS 111 received 1.88 million calls and 88.5% of the calls were answered.
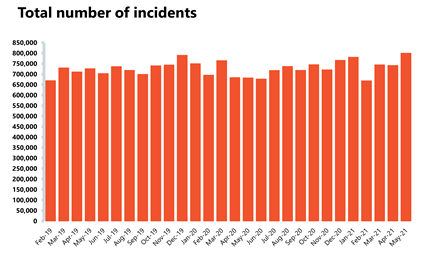
- Ambulance category 1 incidents increased by 16.7% to 67,982 since last month (9,728 more incidents) showing a real jump in activity in the most serious calls.
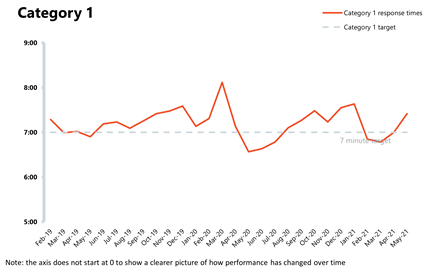
- For the first time in three months the ambulance service missed the average mean response time target of seven minutes for category 1 calls, exceeding it by 25 seconds. The average response time for category 2 calls also deteriorated following pressure on the pathway, with the average mean response time falling to 24 minutes and 35 seconds, missing the 18 minute target.
A&E and emergency care
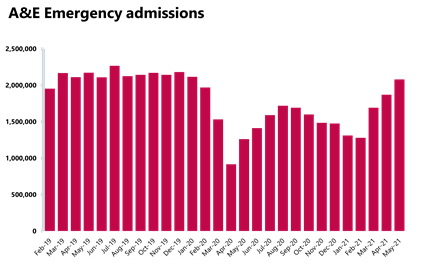
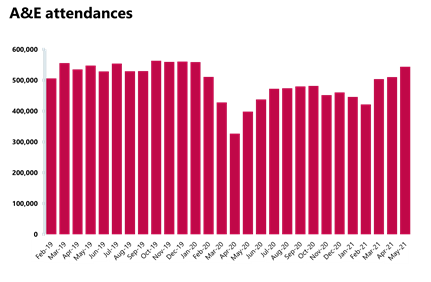
Activity across emergency departments is increasing and activity is back to levels last seen in January 2020.
- In May 2021, there were 2.08 million A&E attendances - the highest figure since January 2020. Attendances increased by 11.2% on the previous month but remain 4% fewer than levels observed in May 2019.
- There were 543,754 emergency admissions in May 2021, an increase of 6.6% since April but 0.7% fewer admissions than in May 2019.
- Performance against the four-hour waiting time target dropped further to 83.7%, missing the 95% standard.
- The number of patients waiting longer than 4 hours has increased this month by 17.6% to 57,307 (8,588 more), while the number of patients waiting more than 12 hours has also increased by 32.7% to 694.
Ambulance category 1 incidents increased by 16.7% to 67,982 since last month (9,728 more incidents) showing a real jump in activity in the most serious calls.
Elective care
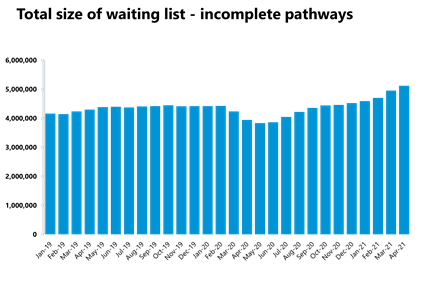
Despite the waiting list exceeding 5 million, inpatient elective care activity has increased again in April 2021, picking up since the January wave. Trusts are now carrying out 95% of elective care activity against the 2019 baseline, exceeding the target of 75% set out by NHS England and NHS Improvement in the 2021/22 planning guidance.
- In April 2021 the size of the elective care waiting list increased by 171,720 to 5.12 million - a 3.5% increase since March 2021. The waiting list is 30% greater than a year ago during the first wave of the pandemic.
- In April 2021, the number of patients waiting more than 18 weeks increased by 2.8% - an additional 48,554 patients - rising to 1.8 million. Performance against the 18 weeks standard remains stable, with 64.6% of people waiting less than 18 weeks.
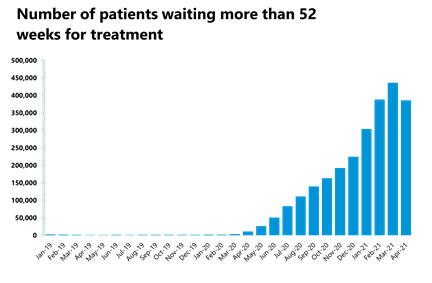
- The number of people waiting over 52 weeks has decreased for the first time in 24 months. The number of long waits fell by 50,637 to 385,490 - a decrease of 11.6%.
- For the first time this month NHS England published data on longer waits of up to 104 weeks. The data shows that a total of 63,152 patients were waiting at least 18 months (78 weeks) for elective treatment. Of these, 10,072 patients were waiting at least two years (104 weeks) for elective treatment.
- To show how widespread long waits are, we looked at the prevalence across trusts. The data shows that 151 trusts had at least one patient waiting at least 52 weeks; 134 trusts had at least one patient waiting at least 78 weeks; and 96 trusts had at least one patient waiting at least 104 weeks. Furthermore, 91 trusts had more than 1,000 patients waiting at least 52 weeks and 13 trusts had more than 1,000 patients waiting at least 78 weeks.
Diagnostics
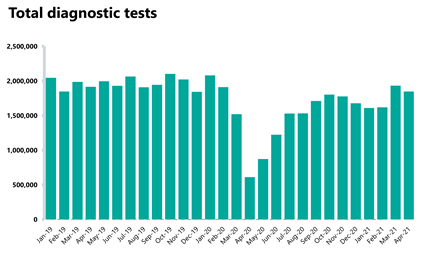
Diagnostic activity is fluctuating and remains a pressure point, potentially impacting on a number of pathways across secondary care.
- The number of tests carried out in April 2021 has decreased by 4.4% to 1.84 million (86,039 fewer). Compared to April 2019, there were 3.6% fewer tests carried out (69,794 fewer).
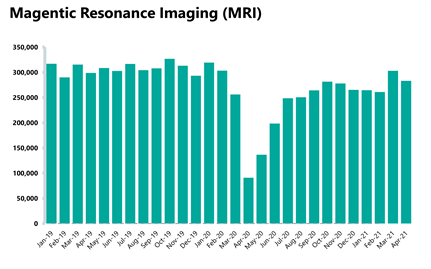
- The number of MRI, CT and colonoscopy tests have all decreased this month, by 6.6%, 3%, and 9% respectively. Compared to April 2020, tests have increased considerably. However, compared to April 2019, the number of MRI tests carried out has decreased by 5.3% but CT scans and colonoscopies have increased by 10.4% and 6.5%.
- The diagnostic waiting list has increased by 3.0% to 1.29 million since the previous month, with 24% of people waiting six weeks or more for a test in April – significantly missing the 1% target again this month.
The waiting list is 30% greater than a year ago during the first wave of the pandemic.
Cancer
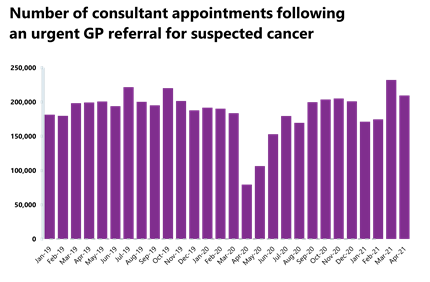
Cancer activity dropped from the high the previous month but remains at pre-pandemic levels for a consecutive month.
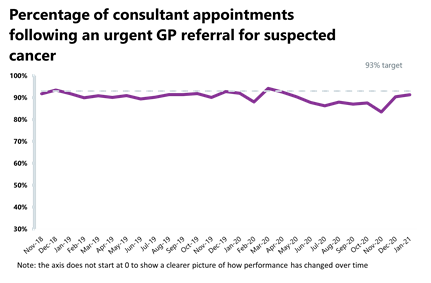
- 209,452 people were seen within two weeks of an urgent referral for a suspected cancer- this is down from the previous month which saw the highest number on record (232,084). This is a decrease of 9.8% since the previous month which means that there were 22,632 fewer consultations. 85.4% of urgent GP referrals were seen within two weeks, missing the 93% standard.
- The number of people on the 31-day pathway, which aims for one month between starting treatment following a decision to treat, also fell this month to 24,963. This is down by 10% since the previous month (2,766 fewer people). 94.2% of people started treatment within one month of the decision to treat, missing the 96% standard.
- The number of people waiting 62 days from urgent GP referral to starting treatment also decreased since the previous month to 13,139. This is 10.5% fewer than the previous month but an increase of 22% since this time last year. 75.4% of the people who started treatment did so within 62 days of their urgent GP referral. This is an improvement from the previous month but it still misses the 85% standard.
Mental health
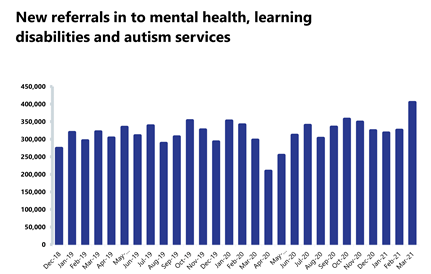
Trust leaders continue to flag the increased pressures on mental health. In March 2021, there were the highest number of referrals reported since records began.
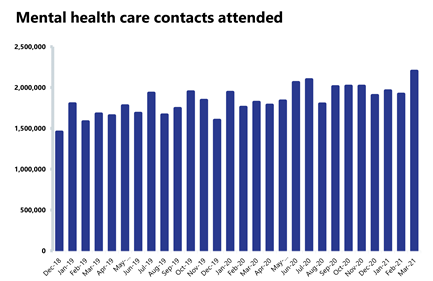
- In March 2021, there were 1.41 million people in contact with mental health services. This is 2.2% more than the previous week and 2.2% more than the same time last year.
- The number of people being referred for mental health services increased by 24.1% to 404,552 since the previous month. This is the highest number of referrals since records began. Compared to last year, referrals have increased by 36% and have nearly doubled since April 2020 (up by 93.7%).
- In March 2021, the number of out of area placements has decreased to 700 (90 fewer OAPs since last month). Compared to April 2020, there are now 245 more OAPs.
- Trust leaders continue to flag the significant increase in demand for mental health services, in particular children and young people’s services.
Our view
Demand increasing across all services
Today's figures reflect the messages from trust leaders that there is increasing demand for physical and mental health services, with the backlog of care left by the pandemic continuing to grow.
Trusts are managing complex situations, with interdependencies across many pathways. For example, a hospital that treats COVID-19 patients carries out planned surgery, provides cancer treatment and has a busy type 1 A&E department, will need to flex how it uses its capacity to treat patients across these pathways. Pressures across urgent and emergency care typically put pressure on bed availability and trusts are put in the unfortunate position of having to cancel operations. The unknown quantity of forthcoming COVID-19 pressures remains a central concern for trust leaders, with indications from the data in the North West and other regions that there may be a more nationwide spike underway.
Worryingly, today's staff absence data also showed that staff sicknesses increased this month, although COVID-19 related absences were lower than last month. However, trust leaders will be acutely aware of the impact increased community prevalence also has on the workforce and we can expect to see associated increases in staff sickness if COVID-19 cases continue to rise.
Given the capacity pressures prior to and during the pandemic, it is vital that trusts can continue to free up as much capacity as possible. Providers are clear that there is a strong case for embedding the discharge to assess model, which has proved so beneficial to patients and their carers over the course of the pandemic. We have published this recent briefing for more information on the discharge to assess model.
Mental health
Today's figures for mental health services show the steep increase in demand, supporting what trust leaders have been telling us for some time. In March trusts received the largest number of referrals for mental health support on record, suggesting that we are perhaps only beginning to see the longer term impact of the pandemic on people’s mental health.
Trust leaders tell us that more people are requiring services, many of whom are presenting with mental health needs for the first time and often with more severe and complex needs than they would typically see before the pandemic.
Following concerns, we recently carried out a survey of mental health trust leaders for children and young people's (CYP) services. The findings included:
- 100% of mental health trust leaders said that the demand their trust/local systems is experiencing for CYP services is significantly (80%) or moderately (20%) increasing compared to six months ago.
- 85% of trust leaders said they could not meet demand for CYP eating disorder services – the highest result across all services.
- Two thirds of trust leaders said they are not able to meet demand for community CAMHS (66%) and inpatient CAMHS services (65%).
- 84% of trust leaders said the amount of time children and young people are currently having to wait to access treatment for services is significantly (25%) or moderately (59%) increasing compared to waiting times six months ago.
- 83% of trust leaders are extremely (37%) or moderately (47%) concerned about staff wellbeing and current levels of stress and burnout across their CYP services workforce.
The survey findings and figures published today clearly show that the pandemic has significantly impacted mental health services. Efforts to tackle the growing backlog of care left by the pandemic must encompass both physical and mental health care.
83% of trust leaders are extremely (37%) or moderately (47%) concerned about staff wellbeing and current levels of stress and burnout across their CYP services workforce.
NHS Activity tracker
A&E
Cancer
RTT
Diagnostic tests
Ambulance indicators
Mental Health
Case Study: The Dudley Group NHS Foundation Trust
The ophthalmology department at the Dudley Group NHS Foundation Trust before COVID-19 was an incredibly busy and appointment-heavy department, with a large footfall. This meant patients had to physically attend an appointment to address their eye concerns, get seen at appointments that took up a large part of the day, and where staff saw multiple patients back-to-back.
The fact that ophthalmology is one of the busiest departments, accounting for over 8% of all outpatient appointments, shows the scale of the black hole left behind if patients were not seen and left without care. As a result of the pandemic, the glaucoma service was forced to implement new pathways at a faster pace, so that they could still provide much needed care to patients.
To set the scene, prior to the pandemic, patients suffering from glaucoma needed multiple follow-ups requiring them to be seen several times in hospital in a year. This meant that patients would attend the hospital for diagnostic tests to check their visual fields, eye pressure and optic nerve health. After undergoing various diagnostic tests, patients were then required to wait to see a consultant for a same-day in-person appointment. At these appointments, consultants would physically check the patient’s eye health. Due to the lengthy nature of these appointments, backlogs of care in the glaucoma pathway were a common occurrence.
The fact that ophthalmology is one of the busiest departments, accounting for over 8% of all outpatient appointments, shows the scale of the black hole left behind if patients were not seen and left without care.
The glaucoma team redesigned the pathways to ensure that patients continued to get regular eye reviews to preserve their sight and ensure good optical health. The pathways were trialled prior to the pandemic in January 2020 but the first wave of the pandemic accelerated the implementation of these.
The new approach meant that patients now attended an off-site diagnostic hub where they underwent all their diagnostic tests. The test results were then uploaded on to the new electronic Medisight system rather than written on paper. Using the results of the diagnostic tests, consultants then conducted a virtual review over the phone or on video with the patients. The new pathway also allowed the purchase of a state-of-the-art 3D camera which meant that physical eye examinations by consultants were no longer necessary and were replaced with the images that the camera took of the patients’ eyes, which were enough to conduct a review.
This new method of delivering crucial glaucoma care has saved patients from attending an incredibly busy acute site which was at the heart of the COVID-19 response, and instead allowed patients to be seen by their consultant in the comfort of their own home, only attending necessary diagnostic tests at the off-site diagnostic hub. The 3D camera has also allowed for shorter appointment times and supports clinical decision making, enabling more patients to be seen and reducing the backlog of consultant appointments. The time it took for patients to be tested has been reduced to 30 minutes where previously this took much longer.
Consultants made sure that patient experience was at the forefront of this innovative virtual method of health care delivery.
The pathways ensured that virtual appointments were still as meaningful and useful to patients as face-to-face appointments. Consultants made sure that patient experience was at the forefront of this innovative virtual method of health care delivery.
The revamped glaucoma pathways allowed for more patients to be seen in the first wave of the pandemic and enabled patients who were overdue a follow up appointment to be seen earlier than they would have previously. The cancellation of surgeries also enabled additional virtual clinics to be conducted, providing more appointment slots. This meant that the department were now seeing 400-600 more diagnostic test and clinician appointments per month. A huge feat and a new method of service delivery welcomed by staff and patients alike.

Babar Elahi, Consultant Ophthalmic Surgeon & Clinical Director
Press Statement
Bearing down on the backlog: trusts are working at full pelt
Responding to the latest monthly combined performance data from NHS England and NHS Improvement, our chief executive Chris Hopson said: "Today's figures highlight just how hard trusts and frontline staff are working. Trusts are going full pelt in elective recovery, now conducting 90% of pre-pandemic levels of operations, well above the 75% target they were set. Positively, the number of people waiting over 52 weeks for treatment to begin fell by 50,000 in a month. But this is in the context of a really significant problem – that the overall waiting list has grown to over five million people.
"Trust leaders are deeply aware of how frustrating long waits for care are, and are doing all they can to prioritise those who need to be seen urgently. They are also worried about the increase in pressures facing the urgent and emergency care pathway, with fears that some patients are now presenting with more complex conditions due to the disruption caused by the pandemic.
"Meanwhile, mental health trust leaders are reporting growing pressure on services, particularly those for children and young people. Activity is also increasing for ambulance and community services, and some hospitals are also grappling with the small spike in COVID-19 cases, particularly in the North West. This is on top of rolling out the national vaccination programme.
"These figures reflect a very busy trust sector operating at full capacity. Urgent and emergency care is under particular strain with ambulances responding to 10% more incidents than two years ago before the pandemic. Hospital bed occupancy also remains high with some trusts now running around 95%, levels typically seen during winter pressures.
"Trusts need more capacity, which the government can commit to through permanent, dedicated funding for discharge to assess. We know that this funding during the pandemic helped free up 30,000 acute beds and improved flow through the system. Its withdrawal would mean increased length of stay for patients, delayed discharges and avoidable readmissions.
"These figures underline once again the extraordinary pressures trust face, and the reality that even a small increase in COVID-19 admissions will impact on other areas activity, including work to tackle the backlog. It’s against that background that decisions over unlocking COVID-19 restrictions will need to be made."