


Introduction
Trusts continue to face ongoing workforce and operational challenges as they take on the demanding task of clearing care backlogs. Staff absences have decreased but continue to be an issue for trusts. For example, between 5 May and 8 June, there were close to 64,000 staff absences, of which 17% were COVID-19 related.
Every month, trusts across England work tirelessly, trying to increase activity across their services to tackle long waiting times in the face of increasing demands. Today's data illustrate once again the remarkable work of NHS staff who endeavour to drive recovery and meet the milestones set out in the recovery plan.
This month's performance figures
Each month, NHS England and NHS Improvement publishes statistics looking at activity and performance across a range of services including urgent and emergency care, routine care, cancer, and mental health. Below we set out the latest trend for each clinical area.
NHS 111: More calls received and more calls answered in April 2022.
- There were an estimated 1,867,856 calls received in April 2022, equating to an average of 62,262 per day. This is an increase of 3,598 calls per day compared to the previous month.
- Of these, 1,490,351 were answered (79.8% of calls received). There were 2.7% more calls received compared to the previous month and 6.3% more calls answered compared to the previous month.
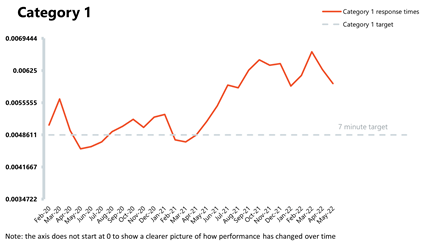
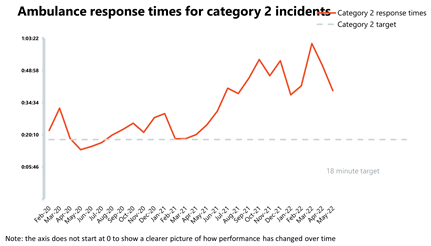
Ambulance: Average response times improved in the face of increased demand across the urgent and emergency care pathway.
- In May, the number of category 1 incidents increased by 1.8% compared to the month before, and were 34.9% higher than three years ago, before the pandemic. The number of category 2 incidents has also increased by 3.3% since April.
- Although national targets are not being met yet, which is indicative of the challenges across the urgent care pathway, the average response time for category 1 and category 2 calls has improved again in May from the previous month by 26 seconds and 12 minutes, respectively.
A&E and emergency care: Pressures continued to be felt in May, which saw the second highest figure on record for A&E attendances, alongside increased emergency admissions.
- There were 2.19 million A&E attendances, a 7.9% increase from April and the second highest figure on record. Emergency admissions increased by 5.6% to 506,693.
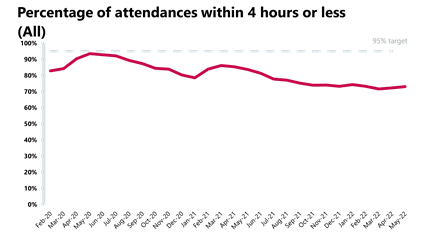
- Although targets for all A&E types were again not met this month, performance has slightly improved.
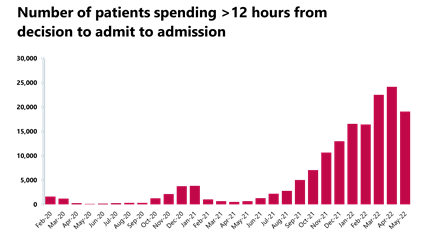
- The number of patients waiting more than 12 hours from the decision to admit to admission decreased to 19,053 (-21%) compared to last month, but this figure is still 4,491% higher than three years ago before the pandemic.
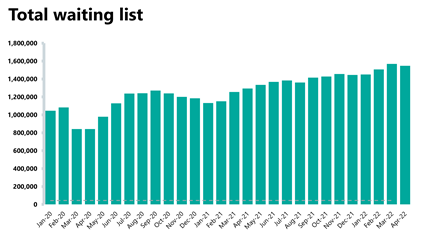
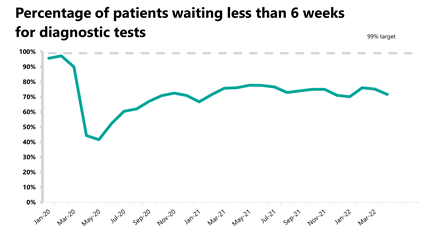
Diagnostics: The waiting list has decreased this month for the first time since December 2021 but remains larger than before the pandemic.
- There were 1.9 million diagnostic tests carried out in April, an 11% decrease from March. Activity is at a similar level to this time last year, with 0.2% more tests carried out compared to April 2021 (3,375 more tests). Activity is lower than pre-pandemic levels, with 66,419 (3.5%) fewer tests being carried out compared to April 2019.
- The numbers of MRI, CT and colonoscopy tests have all decreased compared to the previous month, down by 7.1%, 7.1% and 16.1% respectively.
- The diagnostic waiting list has reduced for the first time since December 2021 and now stands at 1,547,000. This is still 1% lower than the month before (21,914 fewer) but is 20% higher than the same time last year. Compared to April 2019 before the pandemic, the waiting list has grown by 47%.
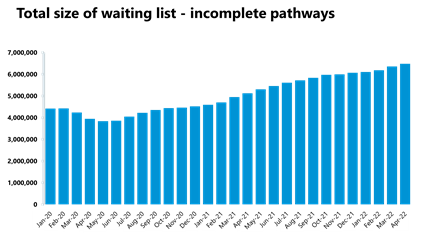
Elective care: The size of the waiting list increased again and remains considerably higher than pre-pandemic levels, but the number of those waiting more than 104 weeks has decreased for the third consecutive month.
- In April 2022, the size of the waiting list increased again to 6.48 million (a 2% increase on the previous month). The size of the waiting list is now 50.8% greater than three years ago before the pandemic.
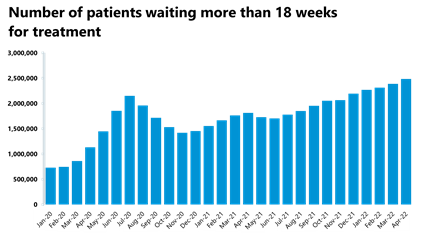
- The number of those waiting more than 18 and 52 weeks has increased again by 4% and 5%, respectively. However, the number of those waiting more than 104 weeks has decreased for the third consecutive month by 24% to 12,735, a reflection of the positive progress towards meeting key national targets.
- Inpatient care activity has decreased in April 2022, with fewer admitted and non-admitted inpatient pathways.
Cancer: Activity for all cancer pathways has decreased compared to the previous month but two-week pathway (urgent referral) activity is now slightly higher than before the pandemic.
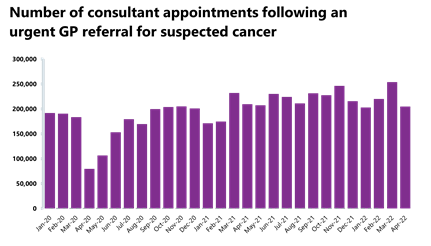
- In April 2022, 204,818 people were seen within two weeks of an urgent referral for a suspected cancer pathway. This is 19.3% lower than March 2022 (48,978 fewer appointments). Activity for the two-week pathway is 2.2% lower than this time last year, and 2.8% higher than three years ago before the pandemic.
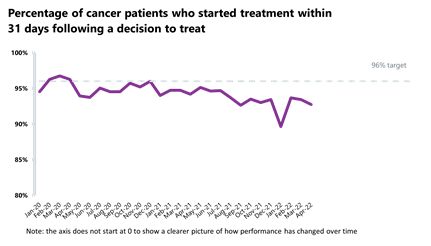
- Activity for the 31-day and 62-day pathways (which aim to start treatment within one month or 62 days from an urgent GP referral) have both decreased from the month before by 8.1% and 4.3%, respectively, and activity is below pre-pandemic levels.
- There were 199,765 patients who completed the 28-day faster diagnosis pathway, which aims to either diagnose or rule out cancer within 28 days of an urgent GP referral for suspected cancer. This is down by 19.6% from March 2022.
- Performance against the waiting time standards has deteriorated across all pathways and the NHS is still missing all key national targets.
Delayed transfers of care: A high proportion of patients continues to remain in hospital despite no longer meeting the criteria to reside, highlighting issues with patient flow and the challenges of getting patients treated closer to or at home.
- On 31 May there were 22,951 patients who no longer met the criteria to reside in hospital. Of these, 52% remained in hospital on that day (11,947).
- For the week commencing 20 May, 97,581 had stayed seven+ days since they met the criteria to be discharged, 89,044 had stayed 14+ days, and 76,577 had stayed 21+ days.
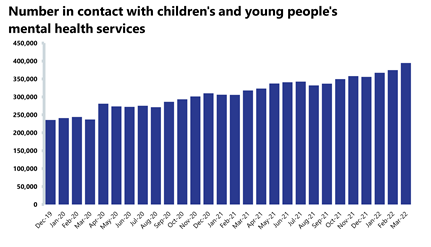
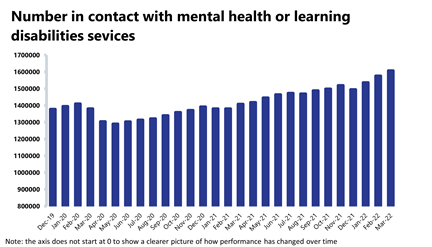
Mental health: Demand continues to increase, with record numbers of people in contact and being referred.
- The number of people in contact with mental health services rose again in March 2022 by 2% to 1,606,766 (30,946 more people in contact). This is the highest number of people in contact with services since records began. Compared to a year ago, this is up by 14.2% (199,181 more) and up by 16.4% compared to two years ago (226,526 more than March 2020). In comparison to pre-pandemic levels, figures are up by 18.1% (246,774 more than March 2019).
- Mental health referrals have increased by 15.7% to 425,277 (57,683 more referrals). This is the highest figure since records began. Compared to a year ago, referrals are up by 5.1% and up by 42.9% compared to two years ago (March 2020). Compared to pre-pandemic levels (March 2019), referrals are up by 32.4%.
- There were 2.14 million care contacts attended, an increase of 12.9% since last month (245,071 more care contacts). This is the second highest number of care contacts on record.
- There were 165,631 referrals to Improving Access to Psychological Therapies (IAPT) in March 2022. This is an increase of 6.5% since the previous month (10,129 more). Compared to a year ago, referrals are up by 4.1% and two times higher than two years ago. Compared to March 2019, IAPT referrals are up by 12.9%.
- In March 2022, the number of out of area placements (OAPs) fell to 670, a decrease of 17.3% (140 fewer than the previous month). Compared to a year ago, this is down by 4.3% (30 fewer OAPs).
Our view
This month's data have, once again, highlighted the pressure currently felt by trusts throughout the country. Demand is mounting across urgent and emergency care, adding significant strain on the pathway and resulting in long waits for patients.
April and May registered record figures across a number of metrics. For example, we saw soaring numbers of A&E attendances alongside increased emergency admissions, as well as a substantial number of people waiting more than 12 hours to be admitted after the decision to admit. This figure remains very concerning and is still remarkably higher than three years ago before the pandemic. These statistics, alongside a high proportion of patients staying in hospital after no longer meeting the criteria to reside, reflect pressures and challenges with patient flow across the whole of the care and health system.
The pressures experienced in the mental health sector are equally difficult. Ongoing demand pressures exacerbate the existing challenges of balancing urgent with the continued effort to reduce the backlog of care across physical and mental health services.
Despite the challenges, these data also highlighted the extraordinary efforts of NHS staff who continue to deliver high-quality care to more and more people in England. We saw the diagnostics waiting list falling for the first time since December and the number of those waiting over a year for elective care decreased for the third month in a row. Equally, the data showed more calls received and more calls answered by NHS 111, and its importance in enabling access to appropriate care pathways. Although targets are not being met yet, we continue to see small improvements in ambulance response times the past few months, despite the increasing demand.
These figures reflect the complex and challenging issues which the NHS currently faces. Looking ahead, with parts of the country experiencing warmer temperatures, it is likely the demand for urgent care will increase, particularly for the already strained emergency services. We also know, however, we will keep seeing the hard work and drive of NHS staff reflected in these numbers, as well as their exceptional efforts to regain ground lost to the pandemic.
The success of providers in tackling the care backlogs
For this month's case study we feature an episode from our Providers Deliver: Tackling the care backlog series on The Provider Podcast. One trust featured in the episode is King's College Hospital NHS Foundation Trust.
From King's College Hospital NHS Foundation Trust, Clive Kay, chief executive, and Ranjeev Bhangoo, head of neurosurgery, explain how the neurosurgery team is using extra theatre time and capacity to carry out 750 more operations a year for patients with time-critical brain tumours and spinal cord compression to prevent backlogs building. As a result, they have been able to operate on individuals as quickly as before the pandemic and have also increased capacity by 7%. We also hear from Jo, the sister of one of the patients treated at King's, about her and her brother's positive experience: she explains that they did not feel "left on hold" and were as close to the neurosurgery team as before the pandemic.
You can listen to the episode below:
A&E
Cancer
RTT
Diagnostics
Ambulance
Mental health
Health and care system under significant and sustained pressure
Responding to the latest monthly combined performance data from NHS England and NHS Improvement, the director of policy and strategy at NHS Providers, Miriam Deakin said:
"These figures reflect significant and sustained pressures across the health and care system.
"Urgent and emergency care is under particular strain, with a high number of 111 calls, high demand in A&E, and lengthy handover delays.
"With significant delays in discharging patients who are medically fit to go home, or to community settings, there are pressures across the health and care system resulting in delays as a patient moves through their care journey.
"However NHS staff are working extremely hard under these circumstances, and this too, is reflected in today's figures. Waits for diagnostics have reduced, and the number of people waiting over two years for a planned operation has been halved since January – a considerable achievement.
"Staff are doing their best to respond to new demand in mental health and community services as well as maintaining elective, cancer and diagnostic activity.
"But trust leaders remain worried about the weeks and months ahead. Hot weather spells over summer increase demand for care making things more difficult for emergency services, and delayed discharges will continue to be a challenge without sufficient investment in our social care system.
"It will be important for the forthcoming urgent and emergency care strategy to explore a system wide response to these pressures, from preventative measures, to emergency response, hospital admission and after care in patients' homes."