


Introduction
Although the prevalence of COVID-19 in the community continues to decrease, trusts are still facing ongoing operational and workforce challenges alongside the task of clearing huge care backlogs. For example, staff absences have decreased but remain high, with an average of 75,226 staff absences each day between 7 April and 4 May, of which about 30% (22,365) were COVID-19 related.
Trusts across the country are working tirelessly to increase activity across many services and bring down long waiting times, despite increased demands. Today's data show these remarkable efforts from NHS staff as they strive to meet the operational targets that will help drive recovery.
This month's performance figures
Each month, NHS England and NHS Improvement publish statistics looking at activity and performance across a range of services including urgent and emergency care, routine care, cancer, and mental health. Below we set out the latest trend for each clinical area.
NHS 111: More calls received but a greater proportion was answered.
- An estimated 1,818,579 calls were received by NHS 111, equating to an average of 58,663 per day. Of these, 77% were answered. NHS 111 received 15.5% more calls since the previous month but has also answered 9.3% more calls.
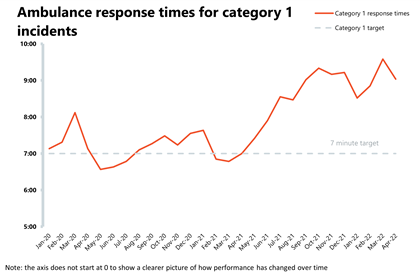
Ambulance: Average response times improved in the face of increased pressures across the urgent and emergency care pathway.
- Category 1 incidents decreased by 6.4% since March, but they are still 31% and 57% higher than one and two years ago, respectively.
- Although national targets are not being met yet, illustrating the real challenges across urgent care, the average response time for category 1 and category 2 calls has improved in April by 33 seconds and by 10 minutes, respectively.
A&E and emergency care: Pressures continue to be felt across urgent care and emergency departments, with high demand and people waiting longer to be admitted after being seen.
- Despite the small 7% decrease from the previous month, A&E attendances were as high as 2.03 million, 121% more than two years ago as the pandemic was starting to have an impact on services.
- Performance against the targets for all A&E types and for type 1 were not met again this week but data showed slight improvements this month.
- The number of people waiting more than 12 hours to be admitted after a decision to admit has increased again, from 22,506 to 24,138, a figure almost 5,000% higher than in April 2019 before the pandemic.
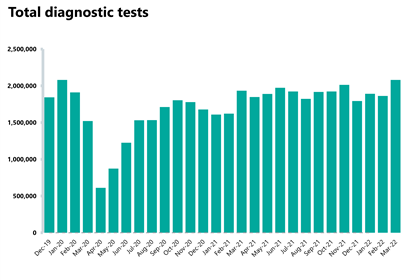
Diagnostics: Highest level of activity for any March on record.
- There were 2.08m diagnostic tests carried out in March, a 12% increase from February. Activity is the highest for any March on record, with 7% more tests carried out compared to a year ago during the pandemic (145,709 more tests). Activity is also higher than pre-pandemic levels, with 92,932 (+5%) more tests being carried out compared to March 2019.
- The number of MRI, CT and colonoscopy tests have all increased compared to the previous month, up by 11%, 11% and 7%, respectively. This month saw the highest number of MRI and CT scans on record.
- Demand remains high with an increase in the diagnostic waiting list (4% higher than the month prior and 46% higher than pre-pandemic levels) and the number of patients waiting six weeks or more for a test has slightly increased to 25%.
Elective care: Demand remains high and has increased from the previous month, but trusts continued to increase elective care activity.
- The size of the waiting list increased again by about 3% to 6.3 million and is now 36% larger than two years ago.
- The number of those waiting more than 18 and 52 weeks has also increased by 3.4% and 2.3%, respectively. That said, the number of those waiting over a year is now almost a third of what was registered one year ago, illustrating the positive progress towards key national targets.
- The number of those waiting more than 104 weeks has decreased to 16,796 from 23,281 observed in February 2022, the first registered decrease since the first record in April 2021.
- Importantly too, inpatient care activity has increased across the board in March 2022, with more admitted inpatient pathways (+14%) and more non-admitted pathways (+14%).
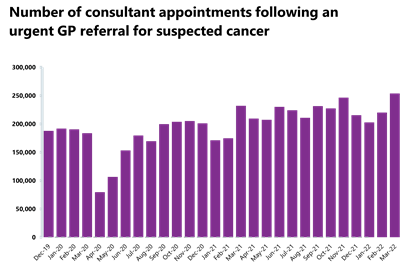
Cancer: Suspected cancer activity continued to increase this month again, exceeding pre-pandemic levels across all pathways, showing the drive to provide care as quickly as possible.
- In March 2022, 253,796 people were seen within two weeks of an urgent referral for a suspected cancer pathway. This is a 15% increase from the month before but also the highest month on record for the two-week pathway. Activity for the two-week pathway is also 27.9% higher than three years ago before the pandemic.
- Activity for the 31-day and 62-day pathways (which aim to start treatment within one month or 62 days from an urgent GP referral) also increased from the month before and is above pre-pandemic levels by 13% and 16%, respectively.
- There were 248,475 patients who completed the 28-day faster diagnosis pathway, aiming to either diagnose or rule out cancer within 28 days of an urgent GP referral for suspected cancer. This is up by 14% from February 2022.
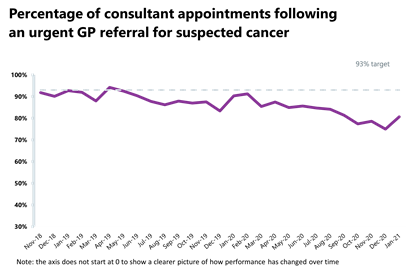
- Performance against the waiting time standards has slightly deteriorated across the two-week, 31-day and 28-day faster diagnosis pathways but has improved for the 62-day pathway.
Delayed transfers of care: A high proportion of patients are remaining in hospital despite no longer meeting the criteria to reside, highlighting issues with patient flow and the challenges of getting patients treated closer to or at home.
- On 30 April there were 20,155 patients who no longer met the criteria to reside in hospital. Of these, 62% remained in hospital on that day.
- For the week commencing 22 April, 105,835 patients had stayed 7+ days since they met the criteria to be discharged, 97,477 had stayed 14+ days and 85,257 had stayed 21+ days.
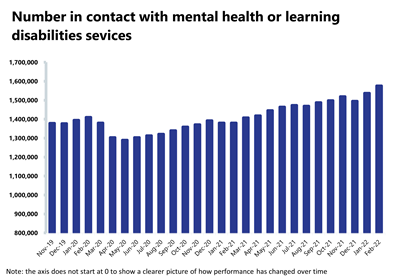
Mental health: Demand continues to soar for the sector, with the highest number of people in contact on record.
- In February 2022, the number of people in contact with mental health services increased again by about 3% to 1,575,820 (39,240 more people in contact). This is the highest number of people in contact with services since records began. Compared to a year ago, this is up by 14% (195,820 more) and 12% (165,991 more) compared to two years ago.
- The number of adult open referrals have increased by 2% to 1,310,460 since the previous month (26,237 more). The number of children and young people open referrals have also increased by 2% to 420,314 (9,182 more).
- Mental health referrals have slightly fallen by 0.8% to 367,594 (3,013 more referrals) but are up by 13% and by 8% compared to one year ago and two years ago (pre-pandemic levels) respectively.
- Referrals to Improving Access to Psychological Therapies services decreased slightly (2%) but remain higher than one year ago (17%) and two years ago (4%).
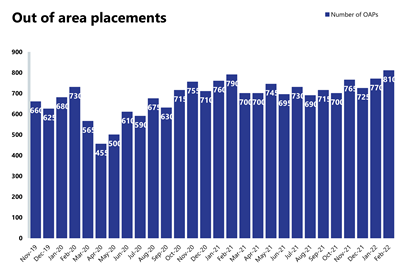
- In February 2022, the number of out of area placements reached 810, an increase of 5% (40 more than the previous month) and the highest figure seen since March 2019.
Our view
This month's data show, once again, how the pressure is continuing to pile up across all NHS services, including urgent and emergency care, community and mental health services. All while the NHS balances COVID-19 care (there were still over 7,000 patients in hospital as of 11 May) with increased non-COVID care and the ongoing effort to reduce the care backlog.
March was the busiest month on record across a number of metrics. There has also been increased demand on the ambulance sector and, by extension, the whole of the urgent and emergency care pathway. This month saw record levels of people waiting more than 12 hours to be admitted after the decision to admit, a concerning figure which is remarkably higher than before the pandemic. These numbers not only signify pressures in urgent and emergency care, but also reflect the challenges with patient flow across the whole health and care system.
Today's data is, however, a powerful testament to the hard work NHS staff continue to deliver. Despite the difficulties, activity levels have improved or been sustained. We are seeing a higher proportion of NHS 111 calls answered even though more calls were received, improved ambulance response times despite increased pressures, A&E performance improving in the face of high demand, elective care activity levels rising, and cancer activity registering all-time records.
These figures highlight the effectiveness and drive of NHS staff, who month after month continue to deliver high-quality care to more and more people across the country, while trying to regain ground lost during the pandemic.
A&E


Cancer
RTT


Diagnostics

Ambulance

Mental health
NHS working flat out for patients but pressures persist
Responding to the latest monthly combined performance data from NHS England and NHS Improvement, the chief executive of NHS Providers, Chris Hopson said:
"It is good to see another drop in the number of people waiting longest for planned treatment. Those waiting more than two years fell for the second consecutive month, and a record number of cancer referrals and more than 2m diagnostic tests were delivered in March.
"Today's numbers show just how effective our hard-working NHS can be as COVID-19 recedes, allowing staff to concentrate more on tackling backlogs and pinch points.
"But pressures on emergency services and the flow of patients persist. A&E departments saw record numbers of people waiting more than 12 hours to be admitted and there are still very significant delays in discharging patients who are fit to continue their recovery closer to or at home, often due to pressures on social care particularly domiciliary care. This has a major, worrying knock-on effect on ambulance services and other parts of the system.
"Mental health services continue to come under strain too with more people in contact with services than ever before, a legacy of the pandemic.
"We must also remember the underlying issues affecting the NHS' ability to provide the right, timely, care to all who need it: the impact of a decade-long financial squeeze; insufficient capacity to meet growing demand; significant staff shortages; and the urgent need to properly fix problems in social care."