Introduction
Today, NHS England published a range of activity and performance data across physical and mental health services. Below we detail the trends across specific services.
This month's data highlight some small dips in activity, albeit remaining above pre-pandemic levels, as well as persistently growing demand across services. As the NHS continues to face workforce shortages and ongoing industrial action, the next few months in the run up to winter will surely present significant challenges.
This month's performance figures
Each month, we look at activity and performance statistics across a range of services including urgent and emergency care (UEC), routine care, cancer, mental health and community services. Below we set out the latest trend for each clinical area.
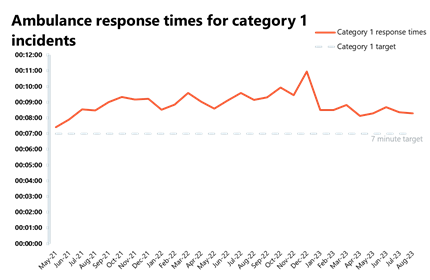
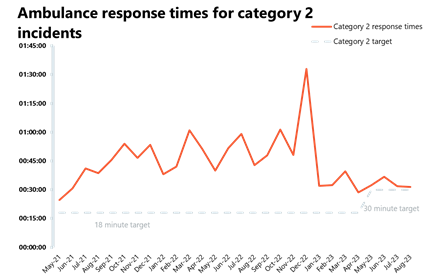
Ambulance activity: Although category 1 incidents decreased from the previous month, it was still a busy August, with this figure nearly 30% higher than before the pandemic. Average response times improved for both category 1 and 2 but are still missing both targets.
- Ambulance category 1 incidents decreased by -2% to 73,826 (-1,895 more incidents). There are nearly 2% more incidents compared to a year ago, and incidents are 28% higher than four years ago, before the pandemic in August 2019. Ambulance category 2 incidents also slightly decreased by -0.8% in August to 376,946 (-3,081 fewer incidents). Compared to four years ago, CT 2 incidents are down by about 2%.
- In August, the average response time across England for category 1 calls decreased by 4 seconds to 8 minutes 17 seconds, missing the 7-minute target, whereas the average response time for category 2 calls also decreased by 20 seconds, reaching 31 minutes 30 seconds, missing the 30 minutes target.
Emergency care activity: August saw fewer A&E attendances compared to last month, but this figure is still over two million, and higher than three years ago. The number of patients waiting more than 12 hours from the decision to admit to admission remains high and increased again this month.
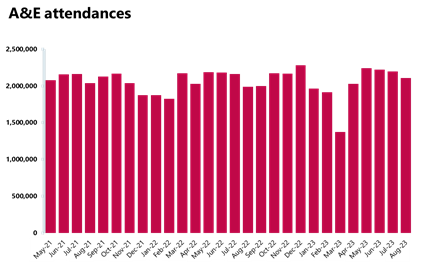
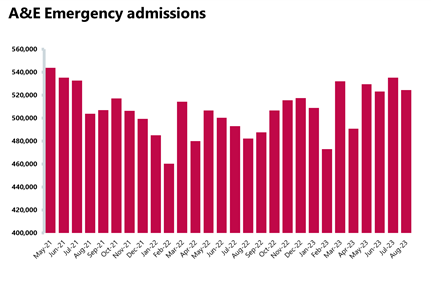
- There were 2,106,146 A&E attendances, a smaller number compared to the month before (-4%), but 22% higher than three years ago. There were 524,467 emergency admissions in July, a 2% decrease on the previous month. However, this figure is about 9% higher than last year (August 2022).
- Performance against the 95% target for all A&E types decreased and it's now 73%. The performance against the type 1 target decreased to 59.1% this month from 60.9%.
- The number of patients waiting more than 12 hours from the decision to admit to admission has increased by about 21% to 28,859 since the month before. This figure is still over 7,600% higher than the same month four years ago before the pandemic (August 2019), when this number was 372.
Elective care: Activity has decreased across the board in July, with the waiting list increasing again, now at an all-time high of 7.7 million.
- The number of admitted inpatient pathways decreased (-8%) with 279,540 inpatient treatments carried out. The number of non-admitted pathways also decreased by nearly 6% on the previous month, and the NHS delivered over 1.1 million (1,146,147) elective non-admitted pathways. The number of new RTT pathways in June also decreased on the previous month from 1.8 million to 1.7 million.
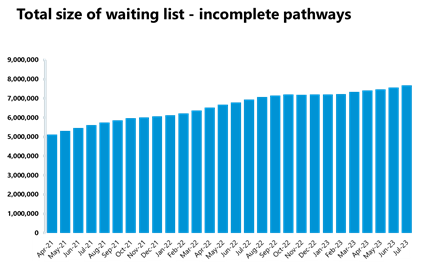
- The size of the waiting list increased again by 1.4% and is now at a record high of 7,679,851 (7.8 million, 105,202 more people than the previous month). The size of the waiting list is still about 70% greater than four years ago before the pandemic.
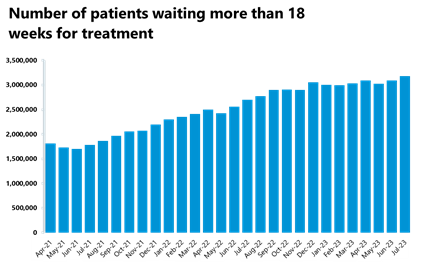
- The number of those waiting more than 18 weeks has increased compared to the previous month (+3%), as did the number of those waiting more than 52 weeks, which is now at 389,952 (+2%). However, the number of those waiting more than 104 weeks has decreased again by around 12% to 277.
- The number of patients waiting more than 78 weeks has increased by 112 patients, and this figure is now at 7,289 (+2%). However, this still represents a decrease of 94% since its peak in September 2021 (124,911) and a decrease of 87% since the start of 2023 (54,882 in December 2022).
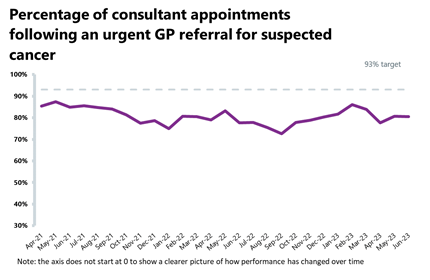
Cancer: Second highest month on record for the two-week urgent referral pathway. Overall, activity is down from the month before, but activity remains higher than pre-pandemic levels. Performance against waiting time standards has deteriorated for the two-week pathway but improved across all other pathways, even if targets are still being missed.
- Over a quarter of a million patients (252,133) completed the 28-day faster diagnosis pathway, which aims to diagnose or rule out cancer within 28 days of an urgent GP referral for a suspected cancer. This is down by 3% from the month before but is 11% higher than the same time last year.
- Over 263,600 patients were seen within two weeks of an urgent referral for a suspected cancer pathway; this is the second highest month on record. Activity in July is up by 1% from June and is above levels seen one year ago (+10%). Activity for the two-week pathway is also above pre-pandemic levels (32% higher than July 2019).
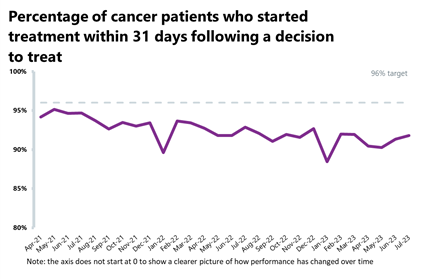
- Nearly 27,650 patients completed the 31-day pathway, which aims to begin treatment within one month from the decision to treat. Activity for this pathway decreased this month, down by 6%. However, this is above levels seen one year ago (+5%) and is above pre-pandemic levels for this month (+8%)
- There were over 15,460 patients who completed the 62-day pathway, which aims to start a first cancer treatment within 62 days from an urgent GP referral. Activity is 4% lower than the previous month but is 9% higher than this time last year and above pre-pandemic levels (14% higher than in July 2019).
- Performance against the waiting time standard has deteriorated for the two-week pathway but improved across all other pathways.
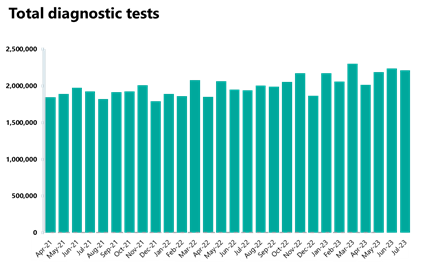
Diagnostics: Third highest month recorded for diagnostic tests carried out (2.21 million), and the waiting list decreased by 1%, even if it still remains 50% higher than before the pandemic.
Activity:
- 2.21 million diagnostic tests were carried out, a decrease of 1% from the month before. This is the third highest month recorded. Activity for the latest month is 14.1% higher than one year ago (274,024 more tests) and is 7% higher than pre-pandemic levels, with 149,644 more tests carried out compared to July 2019.
- The number of MRI and CT scans increased this month, up by 3.2% and 1.2% respectively, but the number of colonoscopies decreased slightly this month by 0.3%. Activity is higher than the same time last year for all MRI (+17%), CT (+13%), and colonoscopy tests (+6%), and all were above pre-pandemic levels, up by 16%, 26% and 14% respectively.
- The diagnostic waiting list decreased this month by 1% to 1,591,413. This is 5% higher than July last year. Compared to July 2019 before the pandemic, the waiting list has grown by 50%.
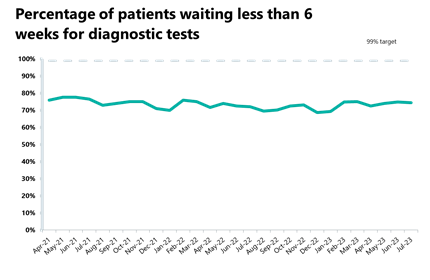
- The number of patients waiting six weeks or more for a test is at 25.5%; this is up slightly from the month before (25.2%) and is still missing the 1% target.
Hospital capacity and discharge: Bed occupancy remains high at 91.8% and over half of patients who no longer met the criteria to reside have remained in hospital.
- In August 2023, there were 98,959 general and acute (G&A) beds available. This is 0.1% fewer beds available compared to the previous month (66 fewer). Of these 91.8% were occupied, down from 91.7% last month. Compared to last year, the number of G&A beds available has increased by 0.9%.
- On 31 August (a Thursday), there were 23,927 patients who no longer met the criteria to reside in hospital. Of these, 49.2% remained in hospital that day.
Community services: Most urgent community response (UCR) teams are meeting their national target, but waiting lists continue to grow.
- As of July 2023, 84% of UCR referrals met the two-hour standard for delivery. This is slightly down from 84.2% in June.
- In July 2023, the total reported waiting list in England was 991,802. This is at a similar level to the month before but is 9% higher than October 2022, when the data collection started. 762,274 of these relate to adult services, a slight increase of 0.3% since the previous month and 8% higher than October 2022. 229,528 of these relate to children and young people's (CYP) services, a decrease of 1.2% since the previous month but 11% higher than October 2022.
- For adult services, 104,642 people have been waiting 18-52 weeks for treatment, an increase of 4.4% since last month. There were 12,350 adults waiting over 52 weeks, an increase of 2.5% since last month. For CYP services, 69,635 were waiting 18-52 weeks, a decrease of 3% since June. There were 18,461 CYP who were waiting over 52 weeks, an increase of 5% since last month.
- On 31 August there were 2,054 patients who no longer met the criteria to reside in hospital. Of these, 85.4% remained in hospital on that day. For the month of August, there were an average of 1,901 patients who no longer met the criteria to reside. Of these, an average of 1,664 (87.5%) patients remained in hospital. This is lower than the previous month (88.3%).
Mental health: Referrals and the number of people in contact increased from the month before and the former are over one third higher than pre-pandemic levels.
- In June 2023, there were 424,645 mental health referrals. This is up by 0.6% compared to the previous month and up by about 11% compared to a year ago. Compared to pre-pandemic levels (June 2019), referrals are up by 37%.
- There were 1,416,169 adult open referrals in June 2023, an increase of 0.5% since the previous month. This is up by 6% compared to a year ago and up by 3% compared to June 2019.
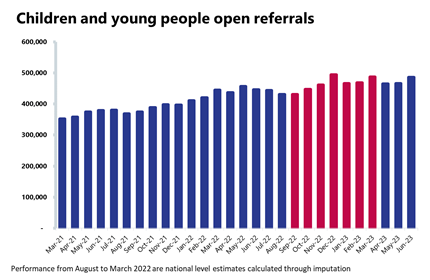
- The number of CYP open referrals is at 486,428, an increase of 4% compared to the previous month (20,178 more) and up by 9% compared to a year ago. This remains considerably higher than June 2019 (80% higher).
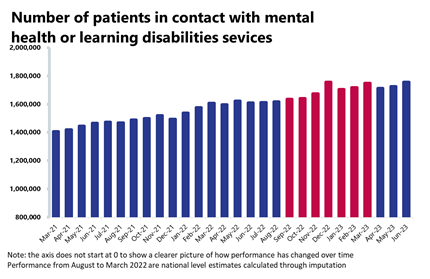
- There were 1,754,522 people in contact with mental health services, an increase of 1.7% since last month. This is up by 9%, compared to a year ago, and up by 28% compared to June 2019.
- There were 143,475 referrals to talking therapies in June 2023, a decrease of 2% compared to the previous month (3,184 fewer referrals). Compared to a year ago, referrals are up by 6% and up by 4% compared to June 2019.
- Nearly 90% of people referred, who finished a course of treatment in the month, accessed NHS talking therapies within six weeks. This is a similar figure to last month's.
- In June 2023, there were 775 out of area placements (OAPs), the same as the previous month. Compared to a year ago, OAPs are up by 20% (130 more).
Our view
The figures from today's data underline once again the enormous challenges facing the NHS across emergency care, hospitals, mental health and community settings. Ongoing industrial action, which has caused nearly one million rescheduled appointments, is undoubtedly adding another layer of operational complexity for trusts at this time. Trust leaders are concerned about the impact of co-ordinated action, as well as the impact continued strikes will have over winter.
The NHS is striving to meet a national plan of UEC recovery, but data continue to demonstrate how demand remains concerningly high. While increases in UEC demand are not unusual during the summer months, this was the busiest summer since before the pandemic, with over 2.2 million A&E attendances in August.
This month, we are also seeing slight decreases in elective care activity, some cancer activity and diagnostics, although some of these remain firmly above pre-pandemic levels. That said, alongside small activity fluctuations, we are noting relentlessly growing waiting lists for elective care and diagnostic tests; with the former reaching an all-time high of 7.7 million patients. This suggests that demand for services is persistently outstripping efforts from frontline staff striving to meet national recovery targets.
Once again, we are seeing significant issues with patient flow, as over half of patients fit to be discharged remain in hospital, at a time when bed occupancy continues to be persistently high, and A&E waiting rooms remain busy, as seen in the number of patients waiting to be admitted after a decision to admit.
But the challenges also exist outside hospitals, with UCR teams meeting national targets, but the waiting lists for community services continually growing, as we see in other sectors. For mental health services, June data published today show how demand continues to be much higher than pre-pandemic levels, and referrals for CYP have increased from the month before as well.
Despite all the obstacles, including worrying workforce shortages and ongoing industrial action, trust leaders continue to focus on the recovery trajectory. Trusts and systems across the country are working to continually increase activity levels, and provide care to as many patients they can. Trust leaders and frontline staff are also now focusing on winter planning and how they will respond to seasonal pressures while sustaining planned care against a backdrop of industrial action.
Integrated Frailty Service wins an NHS Parliamentary Award
Glen Burley, chief executive at South Warwickshire University NHS Foundation Trust, discusses the organisation winning an NHS Parliamentary Award for their Integrated Frailty Service.
We are extremely proud that our Integrated Frailty Service, incorporating acute and community services, won a prestigious national NHS Parliamentary Award in recognition of its innovative and proactive thinking.
The team were chosen as the regional winners in the 'Excellence in Urgent and Emergency Care' category from hundreds of nominations sent by Midlands MPs. Our service then went head-to-head with other regional winners from across the country, before being chosen as the national winner of this category by a panel of senior leaders representing staff and patients from across the country.
The trust's Integrated Frailty Service were presented the award during a ceremony on Wednesday 5 July (the NHS' 75th birthday) at the House of Commons.
The 'Excellence in Urgent and Emergency Care' category recognises outstanding initiatives and exceptional dedication in delivering high-quality urgent and emergency care services within the NHS. The Integrated Frailty Service at our trust has demonstrated remarkable commitment and innovation in addressing the complex healthcare needs of frail individuals in our community.
The service, which works collaboratively with West Midlands Ambulance Service and primary care providers on a range of projects, ensures patients receive the highest level of care in the right place in the first instance – supporting frail older adults in crisis to avoid unnecessary hospital admissions and providing hospital standard care in a patient's home environment.
The team has also received numerous praises nationally for the initiatives they have implemented, which are making a positive impact on patient care and experience. The team are also regularly invited to attend conferences so they can share best practice with other NHS trusts. These initiatives include:
- At the trust, all patients over 75 receive follow-up calls after being discharged from hospital. This scheme has reduced re-attendances from 15% to 3%.
- Urgent community response – community clinician deployed to care for a person experiencing a crisis in their home environment. Response time is two hours maximum, with short-term interventions for up to 48 hours. Referrals are taken from all appropriate sources. On average, this service responds to 800 calls in South Warwickshire a month, preventing unnecessary hospital admissions.
- Same day care services implemented have saved over two wards of beds a year – supporting the trust to have the capacity to care for the people that need inpatient services.
- Using Consultant Connect technology, which enables ambulance crews to talk to a frailty consultant and seek advice. Overall, 50% of these calls meant that a patient did not need to attend the hospital.
- The trust plans to further develop their service by utilising available technology to support an increasing number of specialty patients, who are frail, to receive and manage their care within the community.

Rachel Williams, associate chief operation officer at South Warwickshire University NHS Foundation Trust, said: "It is such an honour to be awarded with a national NHS Parliamentary Award and for our dedication to improving patient care to be recognised in this way.
"Almost 50% of our trust's medical admissions result from patients aged 75+, with 66.5% of all bed days in hospital deriving from this cohort of patients. Hospital is not always the best place for people, with research suggesting caring for a select group of vulnerable older people in their home environment can improve patient outcomes, while reducing pressures on hospitals. By the team boosting care in the community, people receive hospital standard care in the comfort of their own homes – aiding recovery and preventing re-admissions.
"I am extremely proud of our team's ethos to ensure patients receive the highest level of care in the right place first time. This drives us to proactively trial new ways of working, utilise available technology and work closely with our health and social care colleagues from partner organisations."
Adam Carson, managing director at South Warwickshire University NHS Foundation Trust, said: "The national NHS Long Term Plan places huge significance on not just treating people, but also preventing them from getting ill in the first place. Our trust's Integrated Frailty Team has fully embraced this movement. Through innovation, strong leadership, collaborative working and team vision, the service has shifted its culture to prevention by adhering to a home-first mindset.
"This award recognises the team's dedication and tireless efforts to transform the delivery of urgent and emergency care to make a real difference in improving patient outcomes and experience. As an organisation we are extremely proud that our team has been acknowledged in this way."
A&E
Cancer
RTT
Diagnostics
Ambulance
Mental health