Introduction
Today, NHS England published a range of activity and performance data across physical and mental health services. Below we detail the trends across specific services.
This month's data highlight that despite another month of impressive activity gains across many areas, demand persistently outstrips supply across services, contributing to the growth of waiting lists. Moreover, as the NHS continues to face industrial action and workforce shortages, the scenario ahead is one of significant challenge.
This month's performance figures
Each month, we look at activity and performance statistics across a range of services including urgent and emergency care, routine care, cancer, mental health and community services. Below we set out the latest trend for each clinical area.
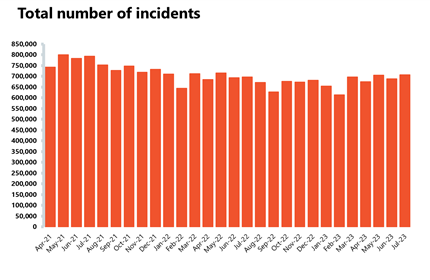
Ambulance activity: A busy July with over 707,000 total incidents, an increase from June, and above levels seen last year (696,000). Average response times improved for both category 1 and 2 but the services are still missing both targets.
- Ambulance category 1 incidents decreased by about 2% to 75,721 (1,342 fewer incidents). There were 11% fewer incidents compared to a year ago, but incidents are over a fifth (23%) higher than four years ago before the pandemic in July 2019. Conversely, ambulance category 2 incidents increased by 3% to 380,027 (12,357 more incidents). Compared to four years ago, these were down by 4%.
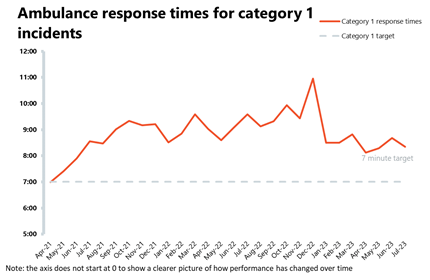
- The average response time across England for category 1 calls decreased to 8 minutes and 21 seconds, whereas the average response time for category 2 calls also decreased to 31 minutes and 50 seconds, both missing the 7- and 30-minute targets, respectively.
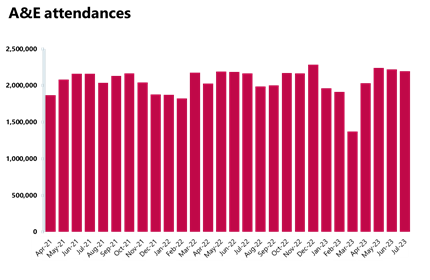
Emergency care activity: Second busiest July ever with over 2.2 million A&E attendances, and the number of patients waiting more than 12 hours from the decision to admit remains high even after another drop of nearly 10%.
- There were 2,220,954 A&E attendances, a slightly smaller number compared to the month before (-1%), but nearly 40% higher than three years ago. There were 525,166 emergency admissions in July, a 2% increase on the previous month. This figure is also 9% higher than last year in July 2022.
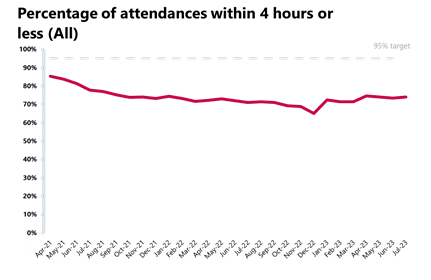
- Performance against the 95% target for all A&E types slightly increased and is now 74.0%. The performance against the type 1 target slightly increased to 60.9% this month from 60.2%, remaining above 60% for the fourth consecutive month.
- The number of patients waiting more than 12 hours from the decision to admit to admission has decreased by 10% to 23,934 since the month before. This figure is still over 5,300% higher than the same month four years ago before the pandemic (July 2019), when this number was 436.
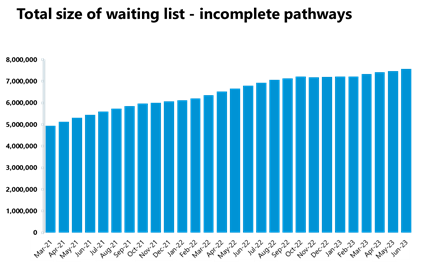
Elective care: Activity has increased across the board in June, but the waiting list increased again too, and is now at an all-time high of 7.57 million showing demand continues to outstrip supply month after month.
- The number of admitted inpatient pathways increased (+5%) with 302,760 inpatient treatments carried out. The number of non-admitted pathways also increased by about 4% on the previous month, and the NHS delivered over 1.2 million (1,217,525) elective non-admitted pathways. The number of new RTT pathways in June also increased on the previous month from 1.7 million to 1.8 million.
- Despite increases in activity compared to last month, trusts have been unable to exceed the baseline activity levels in 2019/20.
- However, in June 2023, the size of the waiting list increased by 1.4% and is now at 7,574,649 (7.57 million, 102,597 more people than the previous month). The size of the waiting list is still 68% greater than four years ago just before the pandemic.
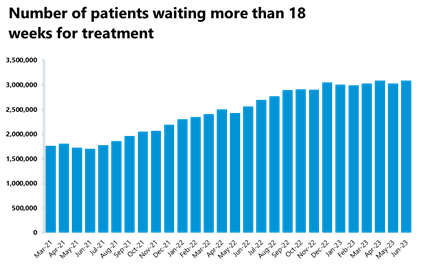
- The number of those waiting more than 18 weeks has increased compared to the previous month (2%). Conversely, the number of those waiting more than 52 weeks slightly decreased and is now at 383,083 (-0.5%). Equally, the number of those waiting more than 104 weeks has decreased again by 35% to 314.
- The number of patients waiting more than 78 weeks decreased by 4,269 patients, and this figure is now at 7,177 (-37%). However, this still represents a decrease of 94% since its peak in September 2021 (124,911) and a decrease of 87% since the start of 2023 (54,882 in December 2022).
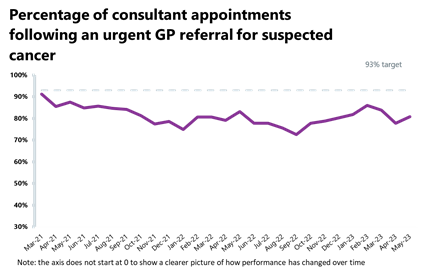
Cancer: Second highest month on record for the two-week urgent referral pathway, all activity is up and performance against waiting time standards improved across all pathways but one, even if targets are still being missed.
- Over 261,000 patients were seen within two weeks of an urgent referral for a suspected cancer pathway, representing the second highest month on record. Activity in June was up by 6% from May and is above levels seen one year ago (+14%) and above pre-pandemic levels (31% higher than June 2019).
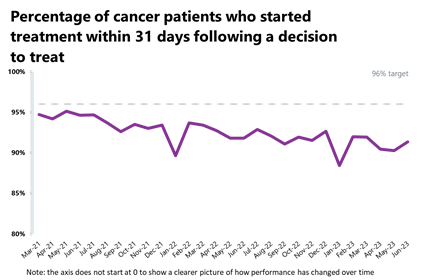
- Nearly 29,500 patients completed the 31-day pathway, which aims to begin treatment within one month from the decision to treat. This is the highest month on record, and is also above levels seen one year ago (+14%) and above pre-pandemic levels (+15%).
- Over 16,000 patients completed the 62-day pathway, the third highest month on record for this pathway, which aims to start a first cancer treatment within 62 days from an urgent GP referral. Activity is 4% higher than the previous month, is 14% higher than this time last year and above pre-pandemic levels (20% higher than in June 2019).
- Lastly, over a quarter of a million patients (259,629) completed the 28-day faster diagnosis pathway, which aims to diagnose or rule out cancer within 28 days of an urgent GP referral for a suspected cancer. This up by 5% from the month before and is 16% higher than the same time last year.
- Performance against the waiting time standard was not met this month – it has slightly deteriorated for the 2-week pathway but improved across all other pathways.
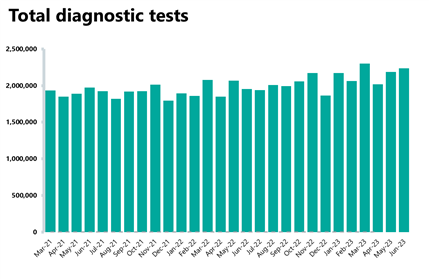
Diagnostics: Second highest month recorded for diagnostic tests carried out (2.24 million), but the waiting list also grew and remains 50% higher than before the pandemic.
- 24 million diagnostic tests were carried out, an increase of 2% from the month before, the second highest month ever recorded. Activity for the latest month is 14.6% higher than one year ago (285,101 more tests) and is 16% higher than pre-pandemic levels, with 308,261 more tests carried out compared to June 2019.
- The number of MRI and CT scans increased slightly this month, up by 0.6% and 0.5% respectively, but the number of colonoscopies decreased this month by 3.5%. However, activity for these three diagnostic tests is also above pre-pandemic levels, up by 18%, 31% and 20% respectively.
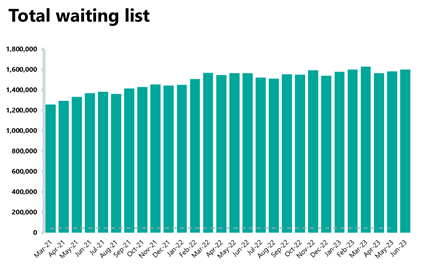
- The diagnostic waiting list increased again this month by 1% to 1,602,033. This is 2% higher than June last year. Compared to June 2019 before the pandemic, the waiting list has grown by 50%.
- The number of patients waiting six weeks or more for a test is at 25.2%; this is down slightly from the month before (25.9%) and is still missing the 1% target.
Hospital capacity and discharge: Bed occupancy remains high at 91.7% and over half of patients who no longer meet the criteria to reside have remained in hospital.
- In July 2023, there were 99,025 general and acute (G&A) beds available. This is 0.9% fewer beds available compared to the previous month (885 fewer). Of these, 91.7% were occupied, down from 92.8% last month. Compared to last year, the number of G&A beds available has increased by 1%.
- On 31 July (a Monday), there were 19,914 patients who no longer met the criteria to reside in hospital. Of these, 56.1% remained in hospital that day. For the month of July, there were an average of 21,697 patients who no longer met the criteria to reside. Of these, an average of 54.7% remained in hospital. This is lower than the previous month (54.8%).
Community services: Urgent community response teams are meeting their national target, but waiting lists continue to grow.
- As of June 2023, 83.5% of urgent community response referrals met the two-hour standard for delivery. This is slightly down from 83.9% in May.
- In June 2023, the total reported waiting list in England was 992,189. This is 2.2% higher than the previous month and 9% higher than October 2022, when the data collection started. 759,837 of these relate to adult services, an increase of 2% since the previous month and 8% higher than October 2022. 232,352 of these relate to children and young people's (CYP) services, an increase of 3% since the previous month and 13% higher than October 2022.
- For adult services, 100,206 people have been waiting 18-52 weeks for treatment, an increase of 0.6% since last month. There were 12,047 adults waiting over 52 weeks, a decrease of 6% since last month. For CYP services, 71,727 were waiting 18-52 weeks, an increase of 7% since May. There were 17,577 CYP who were waiting over 52 weeks, an increase of 11% since last month.
- On 31 July (a Monday) there were 1,960 patients who no longer met the criteria to reside in hospital. Of these, 86.7% remained in hospital on that day. For the month of July, there were an average of 1,933 patients who no longer met the criteria to reside. Of these, an average of 1,708 (88.3%) patients remained in hospital. This is slightly higher than the previous month (87.8%).
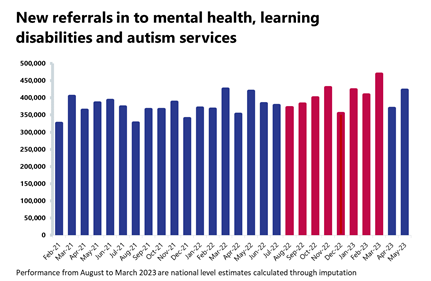
Mental health: Referrals and the number of people in contact with services increased from the month before and remain about one quarter higher than pre-pandemic levels.
- In May 2023, there were 422,190 mental health referrals. This is up by 14% compared to the previous month and up by 0.6% compared to a year ago. Compared to pre-pandemic levels (May 2019), referrals are up by 26%.
- There were 1,409,239 adult open referrals in May 2021, an increase of 0.4% since the previous month. Compared to a year ago, this is up by 6% (82,848 more) and up by 3% compared to pre-pandemic levels (38,521 more than May 2019).
- The number of CYP open referrals is at 466,250, an increase of 0.1% compared to the previous month (447 more) and up by 1.9% compared to a year ago (8,864 more). This remains considerably higher than pre-pandemic levels (71% higher).
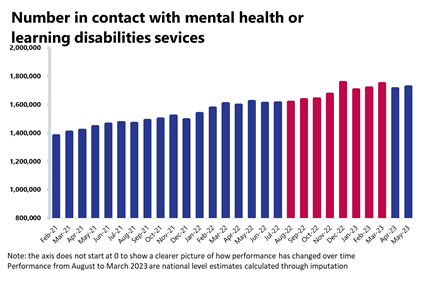
- There were 1,724,697 people in contact with mental health services, an increase of 0.8% since last month. Compared to a year ago, this is up by 6.3% (102,267 more) and up by 25.9% compared to May 2019.
- There were 146,659 referrals to talking therapies in May 2023. This is up by 13% compared to the previous month (16,906 more referrals). Compared to a year ago, referrals are down by 2.3% and up by 1.4% compared to May 2019.
- In May 2023, 90% of people referred who finished a course of treatment in the month, accessed NHS talking therapies within six weeks. This is the same as the previous month.
- In May 2023, there were 775 out of area placements (OAPs), a decrease of 4.9% since the previous month (40 fewer OAPs). Compared to a year ago, OAPs are up 20.2% (130 more).
Our view
Today's figures continue to demonstrate the enormous challenges facing the NHS across emergency care, hospitals, as well as mental health and community settings. Ongoing industrial action and thousands of rescheduled appointments are adding another layer of operational complexity for trusts at this time.
While the NHS endeavours to meet a national plan of urgent and emergency care (UEC) recovery, data suggests that demand remains concerningly high. While increases in UEC demand are not unusual during the summer months, this July saw A&E attendances above levels seen last year and it was the second busiest July ever.
This month, we are again seeing increases in activity across several acute pathways, with the numbers of diagnostics, operations, suspected cancer referrals and those starting cancer treatment all increasing. Once again, this surge in activity, exceeding pre-pandemic levels in several areas, is accompanied by growing waiting lists for elective care and diagnostic tests; with the former reaching an all time high of 7.57 million patients. This suggests that demand for services is persistently outstripping the excellent efforts from frontline staff striving to consistently deliver more.
The data also highlight significant issues with patient flow, as we see over half of patients fit to be discharged remaining in hospital, at a time when bed occupancy remains considerably high, and A&E waiting rooms are consistently busy.
Equally, outside hospitals, we are seeing the urgent community response teams meeting national targets, but the waiting lists for community services continue to grow, as we see in other sectors. For mental health services, May data published today show a particular increase in mental health referrals compared to the month before, a figure that is often higher than pre-pandemic levels.
Despite numerous challenges, such as industrial action and severe workforce shortages, which are hindering the NHS recovery journey, trusts across the country are working tirelessly to recover activity levels, helping as many patients as possible access the care they need.
Sheffield artificial intelligence tool improving cardiac care and waiting times
Kirsten Major, chief executive at Sheffield Teaching Hospitals NHS Foundation Trust (Sheffield Teaching Hospitals), discusses how artificial intelligence is speeding up cardiac diagnosis and improving waiting times.
An award-winning new artificial intelligence (AI) tool developed by staff at Sheffield Teaching Hospitals and the University of Sheffield, is helping to speed up diagnosis and reduce treatment delays for thousands of NHS heart patients.
MRI heart scans are increasingly being used on patients with heart problems to determine how enlarged chambers of the organ are – a sign that it is under strain – and whether they will need invasive surgery or can be treated with medication. The current process for reading these results is time-consuming and resource-intensive, with doctors and cardiac imaging specialists first having to draw contours on the scan images and then undertake complex volumetric and mathematical calculations, to work out blood flow in and out of the heart which shows how well it is functioning. A radiographer can manually process around 10 to 20 scans per day.
The new AI tool – developed in-house by Dr Andy Swift and Dr Pete Metherall takes less than 20 seconds to perform the complex mathematical calculations needed from the scan images. This skips the lengthy manual analysis, meaning radiographers can process more scans each day. In turn, doctors have access to information more quickly, therefore minimising delays and time taken for treatment to begin. They can also spend more time on direct patient care.
It is also the first AI tool to assess the right heart muscle, which is particularly useful in the diagnosis and treatment of pulmonary hypertension, a rare but life-threatening condition. The tool can also process a patient's historical scans, to allow for easier comparison by doctors assessing and managing patients, particularly for those requiring long-term care or repeated scans for treatments.
The technology was extensively tested on thousands of images and validated in over 5,000 anonymised patient scans at Sheffield Teaching Hospitals, with further testing carried out on scans from over 30 hospitals in the UK. The tool has already been rolled out across the trust, with the team now aiming to make it readily available to the wider NHS.
By giving more detailed information on heart function, not only will the tool help improve the early diagnosis in future cardiovascular care, there is also evidence to suggest it could potentially improve care across other treatments and settings, including for cancer patients who are at risk of heart damage from toxic cancer treatments such as chemotherapy and targeted drugs.
Proving more cost-effective and adaptable than commercial software packages, it has saved the trust's radiology department thousands of pounds in subscription fees for commercial software for automated cardiac analysis – something that could be replicated for other NHS trusts.
Since its launch, the tool has won widespread acclaim, including a win at the 2023 NHS Parliamentary Awards and double finalist at the 2023 HSJ Digital Awards. It has also appeared in the prestigious journal, Radiology, and at international conferences, and has received national media coverage.
A&E
Cancer
RTT
Diagnostics
Ambulance
Mental health