What is a sustainability and transformation partnership (STP)?
What is an integrated care system (ICS)?
What about accountable care organisations (ACOs)?
Eight helpful questions for governors to ask
Key points
- This briefing informs governors about how trusts are working collaboratively within health and care systems to make best use of collective resources and improve services for patients. This means focusing on the needs of a local population and overcoming barriers between hospitals, mental and physical health services, local authorities, primary care and the wider public health system, including schools and housing.
- The main vehicles for delivering this strategy are currently sustainability and transformation partnerships (STPs), and integrated care systems (ICSs). This briefing explains what these are and how they are operating.
- Governors may wish to support their trust to work collaboratively in their local health and care system to improve services for patients. Where significant changes for foundation trusts are proposed, governors will need to be consulted as they are now, especially if this falls within the trust’s definition of a significant transaction.
- Governors will therefore be interested in how their NHS foundation trust is contributing to its local STP or ICS, and we provide example questions for governors to ask their board.
- The genuine engagement of patients, communities and NHS staff is crucial to the success of STPs and ICSs. Foundation trust governors are well placed to support trusts’ engagement with the public around STPs and ICSs to ensure that communities, members and the public are engaged in the process.
Introduction
It is now widely accepted that trusts need to work collaboratively within health and care systems to make best use of collective resources and improve services for patients. No trust is an island capable of meeting the health and care needs of the population it serves on its own. This means focusing on the needs of a local population and overcoming barriers between hospitals, mental and physical health services, local authorities, primary care and the wider public health system, including schools and housing.
What is a sustainability and transformation partnership (STP)?
An STP enables NHS organisations, local authorities and clinical commissioning groups to work together to improve the health and wellbeing of a population in a particular area.
Originally described as sustainability and transformation plans, STPs were developed in 44 areas (also known as ‘footprints’) in 2016. Although joint working in STPs is voluntary, every footprint was required to produce an STP plan. STPs were renamed sustainability and transformation partnerships in March 2017 – a longer term vehicle to improve quality of care, tackle health inequalities and reduce the financial deficit.
On the ground, STPs are being used as a catalyst to plan and support discussions about operational collaboration, to help reconfigure services, share workforce and as a means of driving new models of delivering patient care. However, the pace of change varies considerably across the country depending on the quality and history of local relationships, as well as leadership capacity and the various geographical, financial and operational challenges facing the local area.
What is an integrated care system (ICS)?
An ICS was formerly referred to as an accountable care system (ACS), until NHS England and NHS Improvement renamed them in the 2018/19 planning guidance. An ICS is an advanced version of an STP. NHS England has announced the intention for all STPs to become ICSs, although they have not suggested a timeframe for this.
In addition to working together more closely, organisations within an ICS (both commissioners and providers) also take collective responsibility, often in partnership with local authorities, for resources (funding, workforce, estates, technology, information) and population health, either on the STP footprint or, a smaller, sub-STP footprint.
At the time of writing (May 2018), fourteen of the most advanced STPs are evolving into ICSs, including two devolved health and care systems:
• South Yorkshire and Bassetlaw
• Frimley Health and Care
• Dorset
• Bedfordshire, Luton and Milton Keynes
• Nottinghamshire
• Lancashire and South Cumbria
• Berkshire West
• Buckinghamshire
• Greater Manchester (devolution deal)
• Surrey Heartlands (devolution deal)
• Gloucestershire
• Suffolk and North East Essex
• West, North and East Cumbria
• West Yorkshire and Harrogate
The current direction of travel is for ICSs to submit a collective operational plan to NHS England and NHS Improvement (rather than separate organisational plans) and to deliver a shared financial target across organisations within an ICS (known as a ‘system control total’). ICSs are also exploring taking more responsibility for managing collective performance across a system in return for new freedoms and flexibilities in relation to operational performance, some transformation funding, and support from national bodies to develop new ways of working.
What about accountable care organisations (ACOs)?
Considerable media attention has focused on the proposed introduction of ACOs. An ACO within England would occur ‘where the commissioners in that area have a contract with a single organisation for the great majority of health and care services and for population health in the area.’ [NHS England, Next steps on the five year forward view, March 2017]. In practice only two local areas are exploring possible use of this new approach to contracting and delivering services. This briefing therefore focuses on the development of collaborative working in health and care systems through STPs and ICSs as that is relevant across the country.
Governance and engagement
Governors may wish to support their trust to work collaboratively in their local health and care system to improve services for patients. STPs and ICSs have no legal status and derive their decision-making powers from the statutory bodies which comprise them, so an NHS foundation trust board still holds responsibility for decisions in support of the STP. Where significant changes for foundation trusts are proposed, governors will need to be consulted as they are now, especially if this falls within the trust’s definition of a significant transaction.
STPs and ICSs bring together various organisations with different statutory requirements and processes for engaging the public. However plans for change need to follow established public consultation processes, especially as some areas are being asked to consider difficult choices about where best to put resources. The genuine engagement of patients, communities and NHS staff is crucial to the success of STPs and ICSs, as is clinical leadership.
Foundation trust governors are well placed to support trusts’ engagement with the public around STPs and ICSs. Not only do they act on behalf of the interests of the trust’s members and the public, they also have experience in engaging with communities that are traditionally hard to reach, or groups with certain protected characteristics.
Eight helpful questions for governors to ask
Governors will be interested in how their NHS foundation trust is contributing to the STP(s)/ICS, and may wish to consider the following questions:
- What is my trust’s STP/ICS footprint, and who are the key partners in its delivery?
- How is my trust contributing to the STP/ICS, and what is the impact on existing plans?
- How can the council of governors best receive information on progress in delivering the STP/ICS which is relevant to the trust and its patients?
- How will the STP/ICS improve health and care for the local population?
- How can the council of governors best support the trust in leading or contributing to its STP/ICS?
- How is my trust’s STP/ICS getting greater value – better health and care for the population – from the public funds collectively entrusted to providers and commissioners in the footprint?
- What assumptions have been made that underpin the board’s strategy? Has the board actively engaged staff and the public on its plans?
- How can governors support the board to engage with patients and the community around the STP/ICS and any proposed plans for change?
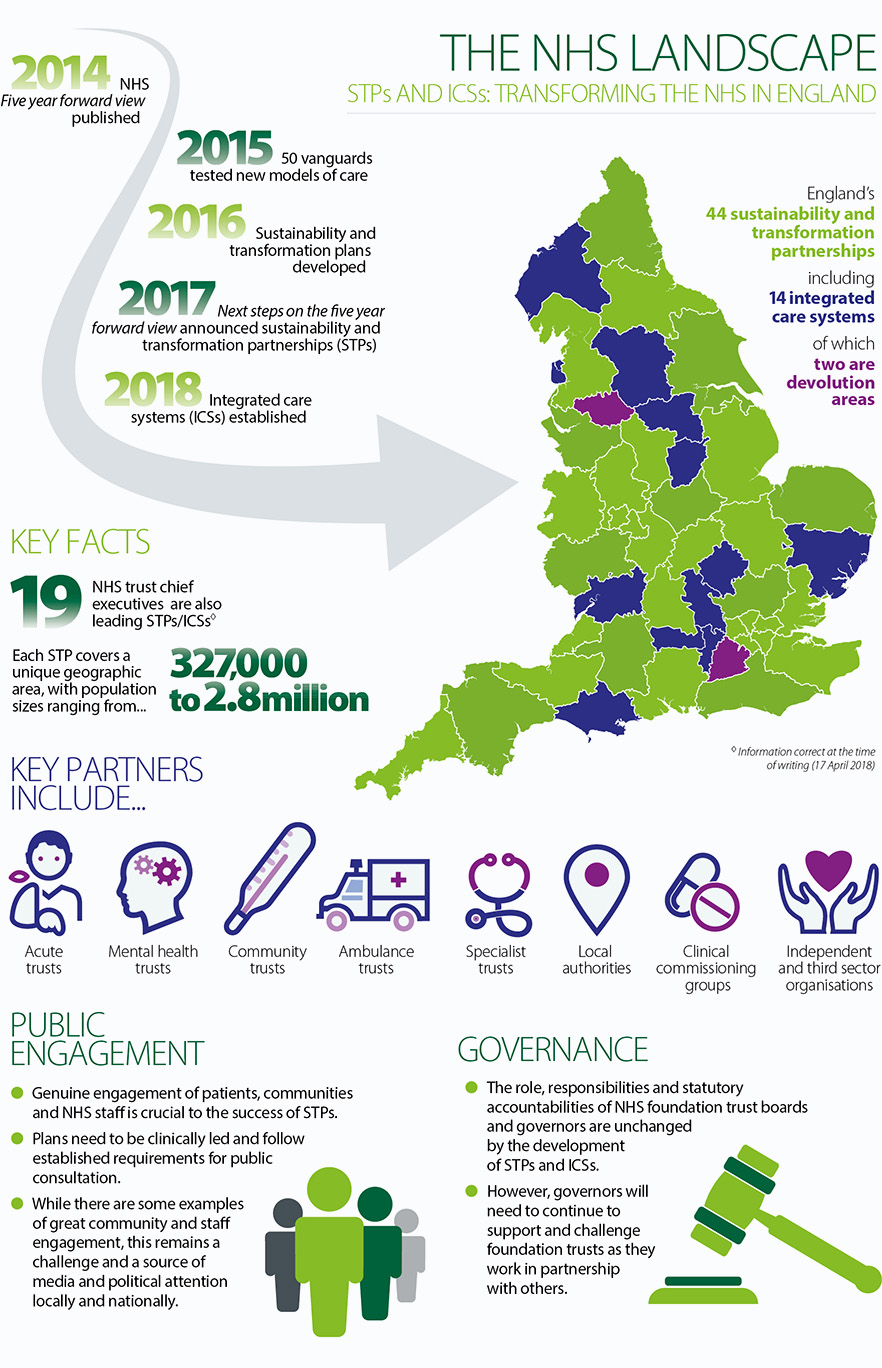
NHS Landscape - infographic
Download this briefing as a pdf to share with your governors.
Related resources
This briefing is part of a series - download our STPs and accountable care background briefing